90 dias, respectivamente). Os pacientes transplantados apresentaram taxas de sobrevida mais elevadas (88,3%). A sobrevida de 4 anos com fígado nativo foi de 36,8%, inversamente correlacionada à idade no momento da portoenterostomia (54, 33,3, 26,6% para < 60,61-90, > 90 dias, respectivamente). Conclusões: Este estudo multicêntrico demonstrou que o encaminhamento tardio das crianças portadoras de atresia biliar ainda é um problema no Brasil, influenciando a sobrevida destes pacientes. Estratégias que proporcionam o encaminhamento precoce estão sendo desenvolvidas com o objetivo de reduzir a necessidade de transplante hepático nos primeiros anos de vida.]]>
90 days, respectively). Higher survival rates were observed among transplanted patients (88.3%). The 4-year native liver survival was 36.8%, inversely correlated with age at portoenterostomy (54, 33.3, 26.6% for < 60, 61-90, > 90 days, respectively). Conclusions: This multicenter study showed that late referral for biliary atresia is still a problem in Brazil, affecting patient survival. Strategies to enhance earlier referral are currently being developed aiming to decrease the need for liver transplantation in the first years of life.]]>
Atresia biliar: a experiência brasileira
Biliary atresia: the Brazilian experience
Elisa de Carvalho1, Jorge Luiz dos Santos2, Themis Reverbel da Silveira2, Carlos Oscar Kieling3, Luciana Rodrigues Silva4, Gilda Porta5, Irene Kazue Miura5, Adriana Maria Alves De Tommaso6, Maria Ângela Bellomo Brandão6, Alexandre Rodrigues Ferreira7, José Roberto de Deus Macêdo8, José Tenório de Almeida Neto8, Grupo de Estudos em Hepatologia Pediátrica do Brasil
1. PhD. Hospital de Base do Distrito Federal (HBDF), Brasília, DF.
2. PhD. Hospital de Clínicas de Porto Alegre (HCPA), Universidade Federal do Rio Grande do Sul (UFRGS), Porto Alegre, RS. ]]>
(1) Articulo original de Brasil, publicado en el Journal de Pediatría (Rio J.) 2010;86:473-9, y que fue seleccionado para su reproducción en la XVI Reunión de Editores de Revistas Pediátricas del Cono Sur -Chile 2011.
Resumo
]]> Objetivo: Avaliar as características epidemiológicas, clínicas e prognósticas de crianças com atresia biliar.Método: Dados sobre portoenterostomia, transplante hepático (TxH), idade no último seguimento e sobrevida foram coletados dos prontuários de pacientes acompanhados em seis centros no Brasil (1982-2008) e comparados em relação às décadas do procedimento cirúrgico.
Resultados: Dos 513 pacientes, 76,4% foram submetidos a portoenterostomia [idade: 60,0-94,7 (82,6±32,8) dias] e 46,6% foram submetidos a TxH. Em 69% dos casos, o TxH foi realizado após a portoenterostomia, enquanto em 31% dos casos o TxH foi realizado como cirurgia primária. Os pacientes da região Nordeste foram submetidos a portoenterostomia mais tardiamente do que as crianças das regiões Sul (p = 0,008) e Sudeste (p = 0,0012), embora, mesmo nas duas últimas regiões, a idade no momento da portoenterostomia tenha sido superior ao desejável. Ao longo das décadas, houve aumento progres si vo do número de TxH realizados. A sobrevida global foi de 67,6%. A sobrevida aumentou nas últimas décadas (anos 1980 versus 90, p = 0,002; anos 1980 versus 2000, p < 0,001; anos 1990 versus 2000, p < 0,001). A sobrevida de 4 anos pós-portoenterostomia, com ou sem TxH, foi de 73,4%, inversamente correlacionada à idade no momento da portoenterostomia (80,77,7,60,5% para < 60,61-90, > 90 dias, respectivamente). Os pacientes transplantados apresentaram taxas de sobrevida mais elevadas (88,3%). A sobrevida de 4 anos com fígado nativo foi de 36,8%, inversamente correlacionada à idade no momento da portoenterostomia (54, 33,3, 26,6% para < 60,61-90, > 90 dias, respectivamente).
Conclusões: Este estudo multicêntrico demonstrou que o encaminhamento tardio das crianças portadoras de atresia biliar ainda é um problema no Brasil, influenciando a sobrevida destes pacientes.
Estratégias que proporcionam o encaminhamento precoce estão sendo desenvolvidas com o objetivo de reduzir a necessidade de transplante hepático nos primeiros anos de vida.
Palabras clabe:
Rev Soc Bol Ped 2012;51 (3): 201-10: Atresia biliar, portoenterostomia hepática, cirurgia, diagnóstico diferencial, prognóstico.
Abstract
Objective: To evaluate epidemiological, clinical and prognostic characteristics of children with biliary atresia.
Methods: Data regarding portoenterostomy, liver transplantation (LTx), age at last follow-up and survival were collected from the records of patients followed up in six Brazilian centers (1982-2008) and compared regarding decades of surgery.
]]> Results: Of 513 patients, 76.4% underwent portoenterostomy [age: 60-94.7 (82.6±32.8) days] and 46.6% underwent LTx. In 69% of cases, LTx followed portoenterostomy, whereas in 31% of cases LTx was performed as the primary surgery. Patients from the Northeast region underwent portoenterostomy later than infants from Southern (p = 0.008) and Southeastern (p = 0.0012) Brazil, although even in the latter two regions age at portoenterostomy was higher than desirable. Over the decades, LTx was increasingly performed. Overall survival was 67.6%. Survival increased over the decades (1980s vs. 1990s, p = 0.002; 1980s vs. 2000s, p < 0.001; 1990s vs. 2000s, p < 0.001). The 4-year post portoenterostomy survival, with or without LTx, was 73.4%, inversely correlated with age at portoenterostomy (80, 77.7, 60.5% for < 60, 61-90, > 90 days, respectively). Higher survival rates were observed among transplanted patients (88.3%). The 4-year native liver survival was 36.8%, inversely correlated with age at portoenterostomy (54, 33.3, 26.6% for < 60, 61-90, > 90 days, respectively).Conclusions: This multicenter study showed that late referral for biliary atresia is still a problem in Brazil, affecting patient survival.
Strategies to enhance earlier referral are currently being developed aiming to decrease the need for liver transplantation in the first years of life.
Key words:
Rev Soc Bol Ped 2012; 51 (3): 201-10: Biliary atresia, portoenterostomy, hepatic, surgery, diagnosis, differential, prognosis.
Introdução
A atresia biliar (AB), caracterizada pela obliteração dos ductos biliares extra-hepáticos, constitui a principal indicação de transplante hepático (TxH) em crianças1. A AB se manifesta nas primeiras semanas de vida e apresenta uma distribuição universal, com incidência variável nas diferentes regiões do mundo2-5. A etiologia da AB ainda não foi completamente elucidada e vários mecanismos têm sido propostos para explicar a colangiopatia progressiva observada nesta entidade6,7. O diagnóstico precoce da AB e o tratamento cirúrgico (portoenterostomia), que restabelece o fluxo biliar, realizados preferencialmente antes dos 60 dias de vida, são fundamentais, uma vez que o diagnóstico tardio relaciona-se a necessidade de TxH ou morte nos primeiros 3 anos de vida8-10. O prognóstico dos pacientes com AB tem melhorado nas últimas décadas, atingindo sobrevida de 90% dos casos 10, devido à realização da portoenterostomia em idade adequada e do TxH seguido de imunossupressão. Mais de 50% dos pacientes submetidos a portoenterostomia tornam-se anictéricos e, entre eles, muitos chegam à adolescência sem TxH. Para aqueles que apresentam complicações como hipertensão portal e cirrose, o TxH proporciona uma boa qualidade de vida11. Vários países têm descrito suas experiências em relação à AB5,12-17, porém há poucos relatos isolados sobre a experiência com AB no Brasil18,19. O presente estudo te ve como objetivo avaliar as características clínicas, epidemiológicas e prognósticas de crianças brasileiras portadoras de AB.
]]> Pacientes e métodos
Neste estudo, foi realizada a avaliação retrospectiva dos prontuários dos pacientes portadores de AB, acompanhados entre julho de 1982 e dezembro de 2008, em seis centros de referência no Brasil: Hospital de Clínicas de Porto Alegre da Universidade Federal do Rio Grande do Sul (UFRGS), região Sul; Hospital Sírio Libanês e Hospital do Câncer, São Paulo, região Sudeste; Universidade Federal da Bahia (UFBA), região Nordeste; Hospital de Base do Distrito Federal (HBDF), região Centro-Oeste; Universidade de Campinas (UNICAMP), região Sudeste; e Universidade Federal de Minas Gerais (UFMG), região Sudeste.
Os dados coletados incluíram: sexo; local de origem (região do Brasil) e categoria da cidade (capital ou interior); peso ao nascer; data de nascimento; início da icterícia; data da internação; presença de anomalias congênitas extra-hepáticas associadas; resultados de exames laboratoriais, ultrassom de abdome, cintilografia de vias biliares, biópsia hepática e do porta hepatis; e os achados cirúrgicos. Em relação a terapêutica, foram avaliados os dados relativos a realização, ou não, dos procedimentos cirúrgicos (portoenterostomia e TxH), a data destes e a evolução pós-operatória, até a data do último seguimento. O diagnóstico da AB baseou-se em critérios clínicos, bioquímicos, histológicos, de imagem e cirúrgicos, conforme já estabelecidos6,11.
Os dados foram analisados inicialmente como grupo de estudo único, sendo posteriormente divididos em três categorias, de acordo com a década em que foi realizada a portoenterostomia: anos 1980 (1982-1989); anos 1990 (1990-1999); e anos 2000 (2000-2008). A idade no momento da portoenterostomia foi classificada em quatro faixas etárias: ≤ 60 dias; 61-90 dias; 91-120 dias; e > 120 dias. Para avaliação da sobrevida global após a PE e da sobrevida com fígado nativo, as faixas etárias compreendidas entre 91-120 dias e > 120 dias de vida foram avaliadas como um único grupo. As informações foram coletadas pelos pesquisadores de cada um dos centros participantes e enviadas ao Centro de Registro de Dados, em Brasília, onde os dados foram inseridos em uma única plataforma para análise estatística. Os pacientes acompanhados inicialmente em um centro e, em seguida, transferidos para outro hospital para a realização de TxH foram considerados como caso único, de apenas um dos centros participantes. Por ser um estudo retrospectivo, não foi possível a coleta completa dos dados de todos os pacientes.
As variáveis categóricas foram descritas em figuras e tabelas de distribuição de frequências e as variáveis contínuas como média ± desvio padrão (DP) ou mediana e intervalo interquartil (IQ). O teste do qui-quadrado e o teste t de Student foram usados para as comparações. As curvas de sobrevida foram construídas pelo método de Kaplan-Meier e pelo modelo de Cox, sendo comparadas pelo cálculo da razão de risco. A sobrevida global baseou-se na data de nascimento e na data do óbito ou do último seguimento. A sobrevida com fígado nativo baseou-se na data de nascimento e na data do TxH, do óbito ou do último seguimento. O nível de significancia foi estabelecido em p < 0,05. O programa Microsoft Excel 2007 (Microsoft Corp, Redmond, WA, EUA) e o programa SPSS versão 15.0 (SPSS Inc, Chicago, IL, EUA) foram utilizados para processamento dos dados e análise estatística.
Este estudo foi aprovado pelos Comitês de Ética em Pesquisa das instituições participantes.
Resultados
Os centros participantes da pesquisa enviaram os dados dos pacientes portadores de AB incluídos no presente estudo (n = 513, 283 do sexo feminino e 230 do sexo masculino) para o Centro de Registro de Dados, em Brasília. O número de pacientes enviados por cada serviço foi: 187 (36,5%), UFRGS; 151 (29,4%), Hospital Sírio Libanês e Hospital do Câncer; 63 (12,3%), UFBA; 53 (10,3%), HBDF; 37 (7,2%), UNICAMP; e 22 (4,3%), UFMG. A distribuição dos pacientes de acordo com as regiões do Brasil foi: 185 (36,1%), Sul; 169 (32,9%), Sudeste; 96 (18,7%), Nordeste; 50 (9,8%), Centro-Oeste; e 13 (2,5%), Norte. Quarenta e cinco (8,8%), 133 (25,9%) e 335 (65,3%) pacientes foram admitidos nos anos 1980, nos anos 1990 e após o ano 2000, respectivamente.
O peso médio ao nascer dos pacientes foi de 3.138,6 (±499,3) gramas e o início da icterícia ocorreu aos 12,3 (±17,0) dias de vida. As anomalias congênitas extra-hepáticas foram encontradas em 61 (11,8%) pacientes, incluindo alterações esplênicas (n = 10), gastrointestinais (n = 25), cardiovasculares (n = 25), urinárias (n = 6) e teratoma (n = 1). Seis pacientes apresentaram mais de uma anomalia. Os achados relacionados a síndrome de malformação esplênica associada a AB ocorreram em 17 pacientes, incluindo poliesplenia (n = 5), situs inversus abdominal (n = 11) e dextrocardia (n = 1).
]]> Os exames laboratoriais demonstraram: bilirrubina total, 11,9 (±6,2) mg/dL; bilirrubina direta, 9,1 (±5,8) mg/dL; gama-glutamiltransferase (GGT), 15,2 vezes o valor normal (x N) (±16,4); aspartato aminotrans-ferase (AST), 6,1 x N (±4,7); e alanina aminotrans-ferase (ALT), 4,7 x N (±4,8). Em relação à histopatologia hepática, a maioria dos pacientes apresentou plugs biliares (93,8%), proliferação ductular/ductal (93,8%) e fibrose (84,1%). Por ser um estudo retrospectivo, não foi possível a coleta completa de dados de todos os pacientes. Os resultados da cintilografia de vias biliares e do ultrassom abdominal, entre outros exames, não puderam ser analisados.Portoenterostomia
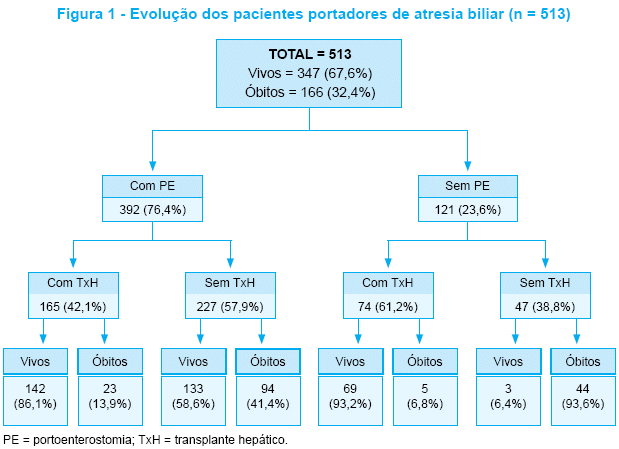
A portoenterostomia foi realizada em 392 (76,4%) pacientes, não sendo possível determinar a idade no momento da portoenterostomia em 12 destes casos (Figura 1).

Estes pacientes foram submetidos ao TxH e a evolução pós-transplante foi avaliada. A idade no momento da portoenterostomia dos 380 pacientes foi 82,6±32,8 dias [mediana = 78,5 (60,0-94,7) dias].
Apenas 100 (26,3%) pacientes foram operados com idade igual ou menor que 60 dias de vida. A maioria dos pacientes (45,0%) foi submetida a portoenterostomia entre 61 e 90 dias, 79 (20,8%) pacientes foram operados entre 91 e 120 dias e 30 (7,9%) pacientes após 120 dias (Tabela 1).

Um número crescente de pacientes foi submetido a portoenterostomia nas três décadas subsequentes deste estudo. Ao comparar a idade dos pacientes no momento da portoenterostomia, foi observado aumento do número de pacientes submetidos ao procedimento entre 61 e 90 dias de vida (p = 0,047) e diminuição após 120 dias de vida (p = 0,020), ao longo das três décadas avaliadas (Tabela 1).
]]> Ao comparar o número de pacientes submetidos ou não a portoenterostomia, de acordo com sua distribuição entre as regiões do Brasil (Tabela 2), a maioria das crianças não operadas era das regiões Norte (69,2%) e Nordeste (45,8%), enquanto apenas 11,9% dos pacientes eram da região Sul. Com relação à categoria da cidade, capital ou interior, não foram observadas diferenças significantes (24,8 versus 23,0%).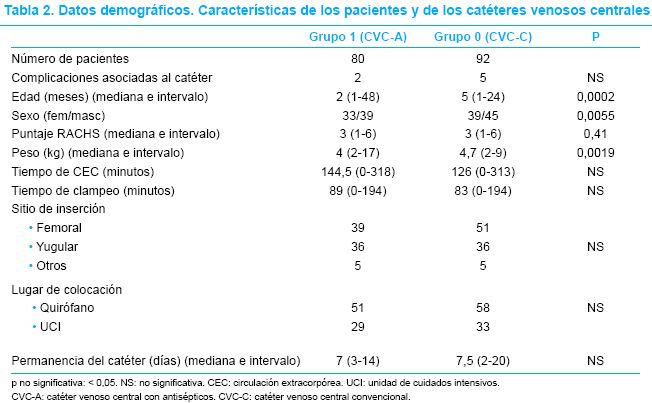
Quanto à idade no momento da portoenterostomia nas diversas regiões brasileiras (Tabela 2), as crianças das regiões Nordeste e Norte foram operadas mais tardiamente [92,3 (±36,1) e 102,2 (±36,4) dias, respectivamente] do que as crianças das regiões Centro-Oeste [84,9 (±29,9) dias], Sul [80,8 (±36,6) dias] e Sudeste [79,5 (±25,4) dias]. A idade no momento da portoenterostomia foi significativamente diferente quando comparadas as regiões Sul e Nordeste (p = 0,008) e as regiões Sudeste e Nordeste (p = 0,012). Entretanto, não foram observadas diferenças entre as outras regiões ou quando os pacientes de capitais [82,2 (±35,9) dias] e do interior [82,8 (±31,3) dias] foram comparados (p = 0,639).
Transplante hepático
Do total de pacientes, 239 (46,6%) foram submetidos ao TxH. A avaliação ao longo das três décadas revelou um aumento progressivo do número de TxH realizados no Brasil (anos 1980 versus 90, p = 0,016; anos 1980 versus 2000, p < 0,001; anos 1990 versus 2000, p < 0,001), conforme descrito na Tabela 1. O TxH foi realizado após a portoenterostomia em 69% dos casos, e como cirurgia primária em 31% dos pacientes (Figura 1). Entre os pacientes previamente submetidos a portoenterostomia, a idade no momento do TxH variou de 0,8 a 2,6 (2,6±3,1) anos. As demais crianças foram transplantadas mais precocemente, em torno de 0,6-1,5 (1,2±0,8) anos, revelando uma diferença significativa entre os grupos (p < 0,001).
Taxas de sobrevida
A sobrevida global foi de 67,6%. Os maiores índices de sobrevida ocorreram nos pacientes transplantados (sem portoenterostomia, 93,2%; com portoenterostomia, 86,1%). A maior taxa de mortalidade ocorreu nos pacientes não operados (93,6%), dentre os quais apenas 3 crianças (6,4%), todas menores de 2 anos de idade, permaneciam vivas na época da pesquisa (Figura 1). A sobrevida global dos pacientes transplantados (88,3%) foi superior à dos pacientes não transplantados (49,6%, p < 0,001). A Tabela 1 demonstra que houve aumento das taxas de sobrevida global, ao longo das três décadas em estudo (anos 1980 versus 1990, p = 0,002; anos 1980 versus 2000, p < 0,001; anos 1990 versus 2000, p < 0,001).
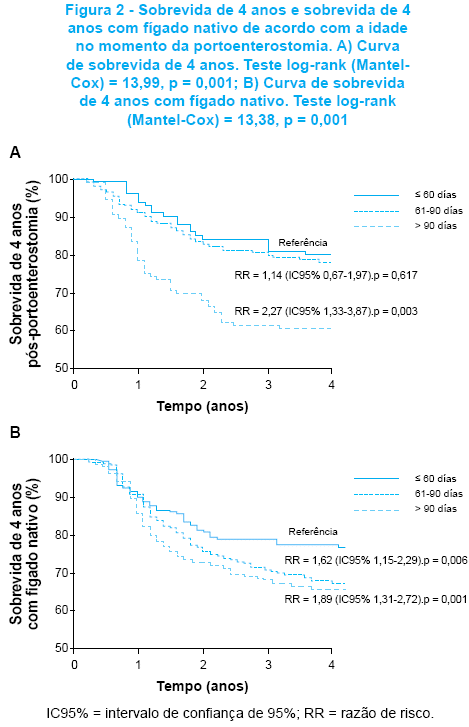
A sobrevida de 4 anos pós-portoenterostomia, incluindo os pacientes transplantados, foi de 73,4%. A Figura 2 A ilustra que a sobrevida de 4 anos foi inversamente proporcional à idade do paciente no momento da cirurgia, com taxas de 80,0, 77,7 e 60,5% em crianças operadas nas idades de < 60 dias, 61-90 dias e > 90 dias, respectivamente. Houve diferença significante entre a sobrevida de 4 anos das crianças operadas com idade > 90 dias, quando comparadas às daquelas submetidas a PE com idade < 60 dias e 61-90 dias (p = 0,003).
]]>
A sobrevida com fígado nativo variou de 0,8 a 3,2 (3,24±4,48) anos. Entre os pacientes que foram a óbito, essa taxa variou de 0,8 a 1,7 (2,0±3,0) anos; nos pacientes transplantados, de 0,7 a 2,0 (2,1±2,7) anos; e naqueles que permaneciam vivos com fígado nativo, este índice foi de 1,3 a 10,7 (6,4±6,2) anos.
A Figura 2 demonstra que a sobrevida de 4 anos com fígado nativo chegou a 36,8% dos casos, apresentando-se inversamente correlacionada à idade no momento da portoenterostomia: 54.0% nas crianças operadas com idade igual ou menor que 60 dias de vida, 33,3% nas operadas entre 61 e 90 dias e 26,6% nos pacientes submetidos a PE após 90 dias de vida, com diferenças significativas entre as faixas etárias (< 60 versus 61-90 dias, p = 0,006; < 60 versus > 90 dias, p = 0,001).
Discussão
Este estudo compreende uma série grande de crianças com AB, que incluiu pacientes de todas as regiões brasileiras, e avaliou os dados relativos a portoenterostomia, ao TxH e à sobrevida. Nesta série, constatou-se um leve predomínio de crianças do sexo feminino (1,2:1,0), em concordância com a literatura20, e um baixo índice de malformações congênitas associadas (12%), indicando, conforme observado em outros estudos21, a prevalência da forma perinatal da AB.
Esta pesquisa demonstrou que, atualmente no Brasil, os pacientes, em sua maioria, não são operados ou são submetidos a portoenterostomia tardiamente, após 60 dias de vida, situação que influencia negativamente na sua sobrevida com fígado nativo. A idade observada, no momento da portoenterostomia, foi superior à desejável, revelando o encaminhamento tardio, um problema já descrito anteriormente em nosso país18,19. Desse modo, no Brasil, o encaminhamento tardio dos pacientes com AB para portoenterostomia continua sendo um problema a ser resolvido em nível nacional, independentemente da região ou da categoria da cidade, seja capital ou cidade do interior. O encaminhamento precoce dos pacientes para realização de portoenterostomia em tempo adequado, continua sendo um desafio em todo o mundo22-26, embora já venha sendo observado em alguns países27, uma tendência de redução da idade no momento do encaminhamento ao longo dos anos. Em países desenvolvidos, a idade no momento da portoenterostomia é de aproximadamente 60 dias13,14,28.
A taxa de sobrevida de 4 anos entre os pacientes brasileiros submetidos a portoenterostomia (73,4%) foi semelhante à observada em outros centros, como no Canadá (79,0%)5 e França (75,3%)13. A taxa de sobrevida de 4 anos com fígado nativo de pacientes brasileiros (36,8%) foi semelhante à dos pacientes canadenses (36,0%)5 e suíços (37,4%)15, porém menor do que a observada no Reino Unido (51,0%)14 e no Japão (63% em 5 anos)28.
Neste estudo, a taxa de sobrevida de 4 anos e a taxa de sobrevida de 4 anos com fígado nativo estiveram inversamente correlacionadas à idade da criança no momento da portoenterostomia, reforçando o efeito negativo da idade avançada no prognóstico pós-operatório8,26,29. Sabe-se que a idade no momento da portoenterostomia influencia na sobrevida com fígado nativo e, segundo Serinet et al.30, seu impacto permanece até a adolescência, pois, se todos os pacientes com AB fossem submetidos a portoenterostomia antes de 46 dias de vida, 5,7% de todos os TxH realizados na França em pacientes menores de 16 anos poderiam ser evitados. Os melhores resultados cirúrgicos são obtidos quando o procedimento é realizado nos primeiros 30 dias de vida5. Ainda é discutível se a portoenterostomia deve ser realizada em pacientes com mais de 90 dias de vida. No presente estudo, a sobrevida de 4 anos com fígado nativo dos pacientes operados mais tardiamente, depois de 90 dias, foi de 26,6%, semelhante à observada no Canadá (23,0% em 4 anos)5 e na França (25,0% em 5 anos)31. Além disso, no Reino Unido, a taxa de sobrevida de 5 anos com fígado nativo dos pacientes operados após 100 dias atingiu 45,0%32. Esses dados sugerem que a portoenterostomia deve ser considerada mesmo em crianças em torno de 90 dias de vida, desde que o paciente não apresente doença hepática descompensada e complicações da hipertensão portal.
A importância da portoenterostomia é evidenciada na Figura 1, que demonstra uma taxa de mortalidade de 41,4% no grupo de crianças submetidas a esta cirurgia e não transplantadas, em comparação aos pacientes que não realizaram qualquer procedimento (93,6%). A portoenterostomia pode proporcionar uma sobrevida de 20 anos com fígado nativo para 21,0% dos pacientes33, enquanto a sobrevida com fígado nativo de crianças não operadas com AB diminui drasticamente nos primeiros anos de vida13. Entretanto, a longo prazo, a maioria dos pacientes com AB terão necessidade do TxH34. No presente estudo, 46,6% dos pacientes foram submetidos a TxH, um índice inferior ao observado em outros países, como a Suíça (64,6%)15 e o Canadá (60,0%)5. Os baixos índices de TxH aqui observados podem refletir as dificuldades socioeconômicas e culturais da população em algumas regiões do Brasil, nas quais o acesso aos centros onde o TxH é realizado nem sempre é possível.
]]> Por outro lado, o TxH foi o primeiro tratamento cirúrgico em 31,0% dos pacientes, índice superior ao observado em outros centros2,4,13-15,26,33, possivelmente refletindo o encaminhamento tardio das crianças com AB. Pacientes submetidos a portoenterostomia foram transplantados mais tardiamente (2,6±3,1 anos) do que as crianças não submetidas ao procedimento (1,2±0,8 anos) (p < 0,001), sugerindo ser vantajosa a realização da portoenterostomia como primeira opção de tratamento cirúrgico. Embora a portoenterostomia possa não influenciar no número total de TxH em pacientes com AB ao longo da vida, ela pode adiar a sua realização35.Em países desenvolvidos, a realização sequencial de portoenterostomia e TxH resulta em taxas de sobrevida global em torno de 90,0%36, superiores à observada neste estudo (67,6%). No entanto, houve aumento das taxas de sobrevida ao longo das últimas três décadas, atingindo um índice de 77,6% na última década, valor semelhante ao obtido no Canadá5 e no Japão2. O aumento progressivo da sobrevida coincidiu com o aumento da realização de TxH, que foi possível pelos esforços de colaboração entre os centros incluídos no Sistema Único de Saúde (SUS), onde os transplantes hepáticos são realizados. A Figura 1 demonstra que os pacientes submetidos ao TxH apresentaram menores taxas de mortalidade, e a sobrevida pós-transplante de 88,3%, é semelhante à observada em países como Canadá5, EUA12 e Reino Unido35. Outro fator que pode influenciar negativamente na taxa de sobrevida global, além da dificuldade de acesso ao TxH, é o encaminhamento tardio de pacientes portadores de AB. No Brasil, o encaminhamento tardio de portadores de AB pode refletir a dificuldade de acesso aos centros de referência ou a falta de suspeição do diagnóstico pelos pais e pelos serviços de pediatria não especializados, uma vez que, no início da doença, os pacientes podem apresentar bom estado geral, peso adequado para a idade, e a icterícia pode ser pouco evidente, principalmente nos pacientes de pele escura. Nestes casos, muitas vezes a icterícia é negligenciada, retardando, assim, o diagnóstico. Experiências de outros países têm demonstrado que o encaminhamento destes pacientes pode ser melhorado por meio do aprimoramento nas práticas médicas e pela adoção de políticas de saúde. O Reino Unido adotou uma política de centralização, em 1999, limitando o tratamento de pacientes com AB a três centros de referência14, enquanto a França, em 1997, iniciou um projeto de colaboração entre seus diversos centros nacionais13. Outros países adotaram medidas para aumentar a conscientização da sua população utilizando sinais de alerta e sistemas de triagem para AB, como as campanhas do "Alerta Amarelo"37 e o uso da escala colorimétrica das fezes para identificar a acolia fecal38,39. Dentre todas estas estratégias, a escala colorimétrica das fezes, que define as fezes normais e as suspeitas por um sistema de graduação de cores das fezes, incorporada à Caderneta de Saúde da Criança e entregue a cada recém-nascido, provou ser eficaz e de fácil aplicação40.
Em resumo, este estudo multicêntrico de pacientes portadores de AB demonstrou que, no Brasil, a sobrevida global destes pacientes está abaixo do nível desejado e já atingido por outros grupos, mas os resultados pós-transplante são semelhantes aos obtidos em países desenvolvidos.
Todavia, o número de TxH ainda está abaixo da demanda populacional. A realização precoce da portoenterostomia aumenta as taxas de sobrevida e diminui a necessidade de TxH nos primeiros anos de vida. O encaminhamento tardio dos pacientes com AB continua sendo um problema em todo o Brasil. Atualmente, os hepatologistas pediátricos brasileiros envolvidos com o tratamento das crianças portadoras de AB, em um esforço nacional, estão desenvolvendo estratégias colaborativas a fim de melhorar a situação destes pacientes.
Esses profissionais, em conjunto com a Sociedade Brasileira de Pediatria e o Ministério da Saúde, incluíram o sistema colorido de graduação das cores das fezes à Caderneta de Saúde da Criança, distribuída pelo Ministério da Saúde aos pais de cada recém-nascido e lançaram uma campanha nacional de "Alerta Amarelo" para a conscientização dos pais e dos pediatras sobre a importância do diagnóstico precoce nos casos de colestase neonatal. Além disso, um consórcio brasileiro de pesquisa da AB, nos moldes do americano Biliary Atresia Research Consortium (BARC), foi criado, para manter a vigilância no diagnóstico e na terapêutica das crianças portadoras de AB, por meio de estudos multicêntricos colaborativos sobre etiologia, terapêutica e prognóstico da doença. O desenvolvimento destes projetos de colaboração pode significar o início de uma nova era no manejo da AB no Brasil. A sorte está lançada!
Referências
1. Balistreri WF, Grand R, Hoofnagle JH, Suchy FJ, Ryckman FC, Perlmutter DH, et al. Biliary atresia: current concepts and research directions. Summary of a symposium. Hepatology. 1996;23:1682-92. [ Links ]
2. Nio M, Ohi R, Miyano T, Saeki M, Shiraki K, Tanaka K; Japanese Biliary Atresia Registry. Five- and 10-year survival rates after surgery for biliary atresia: a report from the Japanese Biliary Atresia Registry. J Pediatr Surg. 2003;38:997-1000. [ Links ]
3. Yoon PW, Bresee JS, Olney RS, James LM, Khoury MJ. Epidemiology of biliary atresia: a population-based study. Pediatrics. 1997;99:376-82. [ Links ]
4. McKiernan PJ, Baker AJ, Kelly DA. The frequency and outcome of biliary atresia in the UK and Ireland. Lancet. 2000;355:25-9. [ Links ]
5. Schreiber RA, Barker CC, Roberts EA, Martin SR, Alvarez F, Smith L, et al. Biliary atresia: the Canadian experience. J Pediatr. 2007;151:659-65. [ Links ]
6. De Carvalho E, Ivantes CA, Bezerra JA. Extrahepatic biliary atresia: current concepts and future directions. J Pediatr (Rio J). 2007;83:105-20. [ Links ]
7. Santos JL, Carvalho E, Bezerra JA. Advances in biliary atresia: from patient care to research. Braz J Med Biol Res. 2010;43:522-7. [ Links ]
8. Mieli-Vergani G, Howard ER, Portman B, Mowat AP. Late referral for biliary atresiamissed opportunities for effective surgery. Lancet. 1989;1:421-3. [ Links ]
9. Nio M, Ohi R. Biliary atresia. Semin Pediatr Surg. 2000;9:177-86. [ Links ]
10. Chardot C, Carton M, Spire-Bendelac N, Le Pommelet C, Golmard JL, Auvert B. Prognosis of biliary atresia in the era of liver transplantation: French national study from 1986 to 1996. Hepatology. 1999;30:606-11. [ Links ]
11. Kelly DA, Davenport M. Current management of biliary atresia. Arch Dis Child. 2007;92:1132-5. [ Links ]
12. Shneider BL, Brown MB, Haber B, Whitington PF, Schwarz K, Squires R, et al. A multicenter study of the outcome of biliary atresia in the United States, 1997 to 2000. J Pediatr. 2006; 148:467-74. [ Links ]
13. Serinet MO, Broué P, Jacquemin E, Lachaux A, Sarles J, Gottrand F, et al. Management of patients with biliary atresia in France: results of a decentralized policy 1986-2002. Hepatology. 2006;44:75-84. [ Links ]
14. Davenport M, De Ville de Goyet J, Stringer MD, Mieli-Vergani G, Kelly DA, McClean P, et al. Seamless management of biliary atresia in England and Wales (1999-2002). Lancet. 2004; 363:1354-7. [ Links ]
15. Wildhaber BE, Majno P, Mayr J, Zachariou Z, Hohlfeld J, Schwoebel M, et al. Biliary atresia: Swiss national study, 1994-2004. J Pediatr Gastroenterol Nutr. 2008;46:299-307. [ Links ]
16. Lai HS, Chen WJ, Chen CC, Hung WT, Chang MH. Long-term prognosis and factors affecting biliary atresia from experience over a 25 year period. Chang Gung Med J. 2006;29:234-9. [ Links ]
17. Tiao MM, Tsai SS, Kuo HW, Chen CL, Yang CY. Epidemiological features of biliary atresia in Taiwan, a national study 1996-2003. J Gastroenterol Hepatol. 2008;23:62-6. [ Links ]
18. dos Santos JL, da Silveira TR, Almeida H, Carvalho PA, Cerski CT. Colestase neonatal - atraso no en-caminhamento de crianças para diagnóstico diferencial. J Pediatr (Rio J). 1997;73:32-6. [ Links ]
19. Kieling CO, Santos JL, Vieira SM, Ferreira CT, Linhares AR, Lorentz AL, et al. Biliary atresia: we still operate too late. J Pediatr (Rio J). 2008;84:436-41. [ Links ]
20. Narkewicz MR. Biliary atresia: an update on our understanding of the disorder. Curr Opin Pediatr. 2001; 13:435-40. [ Links ]
21. Sokol RJ, Mack C, Narkewicz MR, Karrer FM. Pathogenesis and outcome of biliary atresia: current concepts. J Pediatr Gastroenterol Nutr. 2003;37:4-21. [ Links ]
22. Sookpotarom P, Vejchapipat P, Chittmittrapap S, Sookpotarom P, Vejchapipat P, Chittmittrapap S, et al. Short-term results of Kasai operation for biliary atresia: experience from one institution. Asian J Surg. 2006;29:188-92. [ Links ]
23. Mshelbwala PM, Sabiu L, Lukong CS, Ameh EA. Management of biliary atresia in Nigeria: the ongoing challenge. AnnTrop Paediatr. 2007;27:69-73. [ Links ]
24. Lee WS, Chai PF, Lim KS, Lim LH, Looi LM, Ramanujam TM. Outcome of biliary atresia in Malaysia: a single-centre study. J Paediatr Child Health. 2009;45:279-85. [ Links ]
25. Sanghai SR, Shah I, Bhatnagar S, Murthy A. Incidence and prognostic factors associated with biliary atresia in western India. Ann Hepatol. 2009;8:120-2. [ Links ]
26. Karrer FM, Lilly JR, Stewart BA, Hall RJ. Biliary atresia registry, 1976 to 1989. J Pediatr Surg. 1990;25:1076-80. [ Links ]
27. Sokol RJ, Shepherd RW, Superina R, Bezerra JA, Robuck P, Hoofnagle JH. Screening and outcomes in biliary atresia: summary of a National Institutes of Health workshop. Hepatology. 2007:46:566-81. [ Links ]
28. Shinkai M, Ohhama Y, Take H, Kitagawa N, Kudo H, Mochizuki K, et al. Long-term outcome of children with biliary atresia who were not transplanted after the Kasai operation: >20-year experience at a children's hospital. J Pediatr Gastroenterol Nutr. 2009;48:443-50. [ Links ]
29. Subramaniam R, Doig CM, Bowen J, Bruce J. Initial response to portoenterostomy determines long-term outcome in patients with biliary atresia. J Pediatr Surg. 2000;35:593-7. [ Links ]
30. Serinet MO, Wildhaber BE, Broué P, Lachaux A, Sarles J, Jacquemin E, et al. Impact of age at Kasai operation on its results in late childhood and adolescence: a rational basis for biliary atresia screening. Pediatrics. 2009;123:1280-6. [ Links ]
31. Chardot C, Carton M, Spire-Bendelac N, Le Pommelet C, Golmard J, Reding R, et al. Is the Kasai operation still indicated in children older than 3 months diagnosed with biliary atresia? J Pediatr. 2001 ;38:224-8. [ Links ]
32. Davenport M, Puricelli V, Farrant P, Hadzic N, Mieli-Vergani G, Portmann B, et al. The outcome of the older (> or =100 days) infant with biliary atresia. J Pediatr Surg. 2004;39:575-81. [ Links ]
33. López Santamaría M, Gámez M, Murcia J, Díez-Pardo J, Vázquez J, Migliazza L, et al. Kasai operation in the age of liver transplantation. Healing or merely palliative technique? Cir Pediatr. 2000;13:102-5. [ Links ]
34. Lykavieris P, Chardot C, Sokhn M, Gauthier F, Valayer J, Bernard O. Outcome in adulthood of biliary atresia: a study of 63 patients who survived over 20 years with their native liver. Hepatology. 2005;41:366-71. [ Links ]
35. McKiernan PJ, Baker AJ, Lloyd C, Mieli-Vergani G, Kelly DA. British paediatric surveillance unit study of biliary atresia: outcome at 13 years. J Pediatr Gastroenterol Nutr. 2009;48:78-81 [ Links ]
36. Chardot C, Serinet MO. Prognosis of biliary atresia: what can be further improved? J Pediatr. 2006; 148:432-5. [ Links ]
37. Mowat AP, Davidson LL, Dick MC. Earlier identification of biliary atresia and hepatobiliary disease: selective screening in the third week of life. Arch Dis Child. 1995;72:90-2. [ Links ]
38. Matsui A, Dodoriki M. Screening for biliary atresia. Lancet. 1995;345:1181. [ Links ]
39. Chen SM, Chang MH, Du JC, Lin CC, Chen AC, Lee HC, et al. Screening for biliary atresia by infant stool color card in Taiwan. Pediatrics. 2006;117:1147-54.
40. Hsiao CH, Chang MH, Chen HL, Lee HC, Wu TC, Lin CC, et al. Universal screening for biliary atresia using an infant stool color card in Taiwan. Hepatology. 2008;47:1233-40.
Correspondência:
Elisa de Carvalho SQSW 300, bloco N, ap 603 - Sudoeste CEP 70673-048 - Brasília, DF ]]>
Tel.: (61) 9984.4058, (61) 3257.1501]]>