
Efeito da posicao do prematuro no desmame da ventilacao mecanica(1)
Effect of preterm infant position on weaning from mechanical ventilation
Letícia C.O. Antunes*, Lígia M.S.S. Rugolo**, Adalberto J. Crocci***
(1) Artículo original de Brasil. Publicado en el Journal de Pediatria (Rio J), 2003; 79(3): 239-44 y que fue seleccionado para su reproducción en la IX Reunion de Editores de Revistas Pediátricas del Cono Sur. Paraguay 2004
Método: de janeiro a dezembro de 1999, urna amostra de 42 prematuros. com peso de nascimento menor que 2.000g. em ventilacáo mecánica na primeira semana de vida. foram, no início do desmame, randomizados em dois grupos: supino (n=21). e prono (n=21). A freqüéncia cardíaca, freqüéncia respiratória, saturacáo de oxigénio e parámetros ventilatórios foram avaliados a cada hora. A duracáo e as complicacóes do desmame também foram avaliadas.
Resultados: em ambos os grupos, a média da idade gestacional foi de 29 semanas, a maioria dos pacientes foi de muito baixo peso ao nascimento, com síndrome do desconforto respirarório, e a mediana da duracáo do desmame foi de 2 dias. Nao houve difcrenca entre os grupos na freqüéncia respiratória, na freqüéncia cardíaca e na saturacáo de oxigénio; entretanto. episódios de dessaturacáo foram mais freqüentes em supino (p=O.009). No grupo prono. os parámetros ventilatórios foram diminuídos mais rapidamente. e a necessidade de reintubacáo foi menos freqüente (4% x 33%). Nao houve efeitos adversos da posicáo prona.
Conclusáo: esses resultados sugerem que a posicáo prona é segura e benéfica durante o desmame da ventilacáo mecánica, e pode contribuir para o sucesso do desmame em prematuros.
Palabras Claves:
J Pediatr (Rio J) 2003;79(3 ):239-44: prematuro, desmame, ventilacáo mecánica, posicáo.
Abstract
Objective: the purpose of this study was to determine the effects of prone positioning on cardiorespiratory stability and weaning outcorne of preterm infants during we aning from mechanical ventilation.
Methods: from January to December 1999, a sample of 42 preterm infants, with birthweight < 2.000 g. mechanically ventilated in the first week of lite, were randomly divided, in the beginning of the weaning process, in two groups according to the position: supine position (n = 21) or prone position (n = 21). Heart rateo respiratory rate , transcutaneous oxygcn saturation and ventilatory parameters were rccorded every one hour. Length af the wcaning process and complications were also assessed.
Results: in both groups the mean gestational age was 29 weeks, most of the patients presented very low birthweight and respiratory distress syndrorne. The mean length of the weaning process was 2 days. There were no differences between the groups regarding respiratory rate, heart rate and transcutaneous oxygen saturation, howevcr, oxygen desaturation episodes were more frequent in supine position (p = 0.009). Ventilatory parameters decreased faster and reintubation was less frequent in the prone group (4% versus 33%). No adverse effects of prone positioning were observed.
]]> Conclusion: these results suggest that prone position is a safe and beneficial procedure during the weaning from mechanical ventilation and may contribute to weaning success in preterm infants.Key words:
J Pediatr (Rio J) 2003;7913 ):239-44: premature, weaning, mechanical ventilation, position.
Há grande questionamento na literatura quanto as posicóes supina e prona dos recém-nascidos (RN). Para o RN de termo sadio, a American Academy of Pediatrics (1992) recomenda que nao seja adotada a posicáo prona, devido a associacáo, observada em vários estudos epidemiológicos, entre a posicáo prona ao dormir e a síndrome da morte súbita infantill-3. Portanto, com base nos conhecimentos atuais, considera-se que, para os RNs de termo sadios, a posicáo prona nao adequada nem segura, e deve ser evitada.
Entretanto, existem alguns benefícios da posicáo prona na mecánica pulmonar, como maior volume corrente, melhor funcáo diafragmática e menor incoordenacáo
toracoabdominal.4,5
Para o prematuro sadio ou mesmo doente, a posicáo prona apresenta vários benefícios na funcáo respiratória, promovendo aumento da oxigenacáo, decréscimo do C02 expirado, melhora da complacencia e da funcáo diafragmática e diminuicáo da assincronia toracoabdominal.4,5
Os efeitos do posicionamento do RN tém sido investigados em diversas circunstancias do período neonatal, mas existe um período crítico, que é o desmame da ventilacáo mecanica, no qual o efeito da posicáo ainda nao foi avaliado. Assim, este estudo foi proposto em prematuros durante o desmame da ventilacáo mecánica, com o objetivo de determinar os efeitos da posicáo prona na saturacáo de oxigénio (SpO2), na freqüéncia respiratória e na freqüéncia cardíaca; na reducáo dos parámetros do ventilador; na duracáo do desmame, freqüéncia de complicacóes e sucesso do mesmo.
]]> Metodos
Este estudo clínico prospectivo e randomizado foi realizado na unidade de terapia intensiva (UTI) neonatal, do Hospital das Clínicas da Faculdade de Medicina de Botucatu-UNESP, no ano de 1999, após a aprovacáo do Comité de Ética em Pesquisa do HC-FMB-UNESP, parecer n° 302/98. Foram estudados RNs prematuros em ventilacao mecánica, cujos pais assinaram o termo de consentimento livre e esclarecido e que preencheram os seguintes critérios de inclusáo:
Os critérios de exclusáo foram:
Dos 43 RNs incluídos, apenas um foi excluído devido ao nao cumprimento do protocolo de estudo. Nenhum RN foi a óbito no período de estudo.
A idade gestacional foi calculada pela data da última menstruacáo de certeza. ou pelo método de New Ballard10.
O início do desmame da ventilacáo mecánica foi definido pela equipe médica quando em funcáo da melhora clínica, radiológica e gasométrica do RN. Com parámetros do ventilador abaixo de 0.5 de fracao inspirada de O2 (FIO2) 20 cmH2O de pressáo positiva inspiratória (PIP) e 40 cpm de freqüéncia respiratoria. mantendo-se o RN estável e com valores gasométricos adequados, ou seja. PaO2=50-70 mmHg e PaCO2=35-45 mmHg. era iniciada a regressáo progressiva desses tres parámetros ventilatórios. Neste momento, foi realizada a randomizacáo do paciente por meio de sorteio de envelopes lacrados, que definiam a posicáo, supina ou prona, que foi adotada até a extubacáo. Foram assim constituídos os dois grupos de estudo: prono n== 21 e supino n== 21. Após a extubacáo, todos os RNs foram posicionados em supino para aplicacáo de 5 cmH20 de pressáo positiva contínua em vias aéreas. por via nasal (CPAPn), e foram avaliados quanto ao sucesso do desmame até 48 horas após a extubacáo, que é um período crítico para a falha na extubacáo11, Nao foi utilizada aminofilina durante ou após o desmame. e a fisioterapia respiratória nao foi realizada de rotina. As técnicas fisioterapéuticas foram realizadas por um fisioterapeuta que desconhecia os objetivos do estudo, bem como do posicionamento: as sessóes tinham duracáo de. no máximo, 20 minutos e consistiam de desobstrucáo brónquica: drenagem postural, percussáo manual e aspiracáo das secrecóes. Foi socilitado pelo médico o pedido de fisioterapia para cinco RNs do grupo supino. e para seis do grupo prono. Os RNs alocados no grupo supino foram mantidos nesta posicáo durante todo o período de estudo. Os RNs do grupo prono eram colocados em supino no período das 7h as 10h para higiene, exame físico, coleta de exames laboratoriais e radiografia torácica. Os dados registrados durante este período nao foram considerados na análise dos resultados.
Os RNs foram monitorizados continuamente quanto a saturacáo de O2 e freqüéncia cardíaca. A freqüéncia respiratória, a freqüéncia cardíaca, a saturacáo de O2 os parámetros do ventilador e as intercorréncias de cada pacient foram avaliados e registrados pela enfermagem a cada urna hora. no protocolo da pesquisa.
Quanto aos parámetros ventilatórios (Fi02, PIP e freqüéncia respiratória do ventilador), foram considerados os valores médios de cada dia e, para as outras variáveis, valorizou-se a ocorréncia. em pelo menos duas avaliacóes ao dia, das seguintes alteracoes:
A presenca de atelectasia foi definida com base no achado da radiografia de tórax, realizada nos casos de dificuldade no desmame e nas primeiras 12 horas pósextubacáo, em todos os RN. A apnéia foi definida como urna pausa inspiratória maior que 20 segundos ou de menor duracáo, mas associada a bradicardia e/ou cianose.
O sucesso do desmame foi definido pela permanencia do RN extubado durante 48 horas pós-extubacáo.
Na comparacáo entre os grupos supino e prono, utilizouse o teste t de Student ou o teste de Mann Withney para as variáveis quantitativas, e o teste do X2ou exato de Fisher para as variáveis categóricas, com nível de significáncia em 5%12.
Resultados
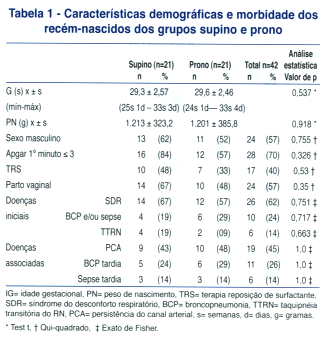
As características demográficas e a morbidade da amostra estudada estáo apresentadas na Tabela 1.
]]>
A mediana da idade no início de desmame no grupo supino situou-se na primeira semana (quatro dias), e no grupo prono na segunda semana de vida (11 dias), sem diferenca estatística. Em ambos os grupos, o tempo de desmame foi breve. com mediana de dais dias (Tabela 2).
Nas primeiras 24 horas do desmame, apenas um paciente em cada grupo pode ser extubado; entre 24 e 48 horas, 57% dos pacientes em cada grupo foram extubados, e, ao término do terceiro dia do processo de desmame, somente tres RNs do grupo supino e um do grupo prono continuavam intubados. Por este motivo, os efeitos da posicáo do RN foram avaliados nos tres primeiros dias do desmame.
Nao houve diferenca nos valores médios da SpO2, (95%x96%). freqüéncia respiratória (48x49) e freqüéncia cardíaca (144x147) nos grupos supino e prono, respectivamente.
O número de pacientes que apresentaram Sp02 < 90% foi significativamente maior no grupo supino, conforme mostra a Figura 1.
No primeiro dia do desmame, tres pacientes do grupo supino e cinco do grupo prono apresentaram taquicardia (p=0,697); episódios de taquipnéia ocorreram em dais pacientes do grupo supino e em cinco do grupo prono (p=0,25 1). Houve diminuicáo destas intercorréncias no segundo dia (apenas dais pacientes em cada grupo tiveram taquipnéia) e desaparecimento no terceiro dia de desmame.
A Tabela 3 mostra que a posicáo do RN nao teve influencia significativa na FiO2, utilizada nos primeiros tres dias do desmame, mas a posicáo prona favoreceu a diminuicáo da PIP e da freqüéncia respiratória do respirador, com diferenca significativa entre os grupos supino e prono.
]]> Na Tabela 4, observa-se que, dentre as cornplicacóes do desmame, as atelectasias predominaram nos dais grupos, sem diferenca significativa entre eles. entretanto, a necessidade de reintubacáo foi mais freqüente no grupo supino (p=0,049). As principais causas de reintubacáo foram as atelectasias, em cinco casos, e apnéia, em dois casos. Nesta amostra, nao ocorreu extubacáo acidental ou qualquer efeito indesejável do posicionamento.
Discussao
As características demográficas dos RNs mostram que os dois grupos de estudo foram homogéneos.
A casuística foi constituída basicamente de prematuros de muito baixo peso, com idade gestacional média de 29 semanas, refletindo o perfil dos pacientes atendidos na un neonatal desta instituicáo. Esta é uma característica importante da amostra, pois estes RNs apresentam elevada morbimortalidade neonatal e grandes limitacóes em sua funcáo respiratória, seja no controle central da respiracáo, na imaturidade anatómica e bioquímica pulmonar e também na mecánica respiratória.13
A idade no início do desmame nao diferiu entre os grupos, mas individualmente houve grande variabilidade em funcáo da morbidade apresentada por estes prematuros na primeira semana de vida. Pode-se dizer que o desmame foi realizado no momento oportuno, pois o tempo de desmame foi relativamente curto, com mediana de dois dias. A duracáo do desmame é pouco referida na literatura, mas há consenso em que a ventilacáo mecánica deve ser mantida pelo tempo mínimo necessário, até que o paciente seja capaz de manter adequadamente sua respiracáo espontánea, A cada dia, estando o paciente estável e com melhora nas trocas gasosas, o médico deve questionar se o paciente é capaz de respirar espontaneamente, evitando assim horas ou dias de ventilacáo desnecessária e suas tradicionais complicacóes.14
A menor ocorréncia de episódios de diminuicáo da SpO2, em prono, no primeiro dia de desmame, pode ser devida a melhora da mecánica respiratória, pois em prono ocorre diminuicáo na assincronia toracoabddominal.8,15
Nao evidenciamos efeito do posicionamento na freqüéncia cardíaca e na freqüéncia respiratória dos prematuros estudados, e, neste aspecto, nao há consenso na literatura. No estudo de Mendonza et al. (1991), os valores de freqüéncia cardíaca foram menores na posicáo prona, enquanto que Sahni et al. (1999) encontraram o inverso, e Lioy & Manginelo (1988) relataram diminuicáo da freqüéncia respiratória nos RNs em prono. Esta variabilidade pode ser decorrente de diferencas na casuística e no método dos estudos.7,16,17
A posicáo prona favoreceu a reducáo mais rápida de alguns parámetros ventilatórios, como a PIP e a freqüéncia respiratória, o que pode ser atribuído a melhora da mecánica respiratória em prono. Este é um resultado importante, que nao havia sido anteriormente investigado na literatura.
]]> O sucesso da extubacáo depende da capacidade do paciente efetuar a respiracáo espontánea e manter adequadas trocas gasosas. Sabe-se que no RN, principalmente no prematuro, a alta complacencia da caixa torácica pode reduzir a eficiencia da ventilacáo, e existe risco maior de falha na extubacáo, quando o esforco respiratório resultar em volume corrente insuficiente, quando houver aumento na carga dos músculos respiratórios, ou quando o controle inspiratório central for insuficiente. A extubacáo associa-se transitoriamente a aumento na carga diafragmática, recrutamento de músculos acessórios e aumento da freqüéncia respiratória, que sao importantes adaptacóes mecánicas para sustentar a ventilacáo minuto e manter os volumes pulmonares. Quando o RN é incapaz de realizar estas adaptacóes, surgem as apnéias, que constituem importante causa de insucesso da extubacáo.11Uma preocupacáo durante o desmame e após a extubacao refere-se a presenca de atelectasia, que causa relativa é mente freqüente de prolongamento e/o u insucesso no desmame da ventilacáo mecánica. Neste estudo, a freqüéncia de atelectasia foi duas vezes maior em supino do que em prono, tanto durante o desmame como após a extubacáo, As atelectasias ocorreram mais freqüentemente em lobo superior do pulmáo direito, podendo estar relacionadas com a mobilizacáo e o mau posicionamento da cánula orotraqueal, causando intubacáo seletiva a direita, além do risco sempre presente de acúmulo de secrecóes nos pacientes intubados. Considerando que o acúmulo de secrecóes em vias aéreas está diretamente relacionado com o tempo de permanencia da cánula traqueal, seria esperado que a ocorréncia de atelectasia fosse maior nos pacientes do grupo prono, cuja mediana da idade de extubacáo foi de 11 dias, enquanto que em supino foi quatro dias: entretanto, a posicáo prona pode ter colaborado para menor movimentacáo dos pacientes, e conseqüentemente, da cánula traqueal18-20.
Após a extubacáo, os RNs deste estudo foram mantidos com pressáo positiva contínua em vias aéreas por via nasal, o que tem sido recomendado, principalmente no recémnascido de muito baixo peso, para prevenir o aparecimento de atelectasias e apnéias e, assim, favorecer o sucesso da extubacáo21 . Apesar destes benefícios esperados, o CPAP nasal nao garantiu o sucesso da extubacáo em todos os pacientes estudados, e 19% da amostra necessitou de reintubacáo nas primeiras 48 horas pós-extubacáo.
Estudo recente com 30 prematuros extremos, para investigar os fatores que predizem falha na extubacáo, mostrou que 1/3 dos prematuros necessitaram de reintubacáo, e a baixa idade gestacional foi o melhor preditor de falha na extubacáo22.
Nosso percentual de falha na extubacáo (19%) está de acordo com o referido na literatura, em que se encontra cifras variáveis, de tres a 19% em adultos, e de 22 a 33% em neonatos prematuros11,22,23. Pode-se dizer que a posicao prona foi benéfica em relacao a este desfecho, pois apenas um paciente do grupo prono foi reintubado, enquanto que sete (33%) do grupo supino necessitaram de reintubacáo, sendo esta diferenca estatisticamente significativa.
A preocupacáo com a falha na extubacáo justifica-se por associar-se com aumento na morbimortalidade e prolongamento do tempo de un e de hospitalizacáo24.
Neste estudo, nao ocorreu extubacáo acidental, ou outras complicacóes mais raras, associadas ao posicionamento prono por tempo prolongado, como edema subcutáneo posicional, edema de face, lesáo de córnea, perda de acesso vascular e úlceras de pressao25,26.
Os resultados deste estudo clínico, realizado com metodologia simples e recursos nao dispendiosos, mostraram que a posicáo prona foi benéfica para prematuros durante o desmame da ventilacáo mecánica, pois favoreceu o sucesso da extubacáo, sem alterar os parámetros fisiológicos e sem efeitos indesejáveis. Assim, consideramos que a posicáo prona pode ser urna boa opcáo para prematuros durante o desmame da ventilacáo mecánica. Novas estudos devem avaliar a eficácia e seguranca deste posicionamento em prematuros, pois os dados atuais disponíveis ainda nao sao suficientes para recomendar o uso rotineiro desta posicáo.
Referencias bibliográficas
1. American Academy of Pediatrics. Task force on infant positioning and SlDS: Positioning and SIDS. Pediatrics 1992;89(6 Pt 1):1120-6. [ Links ]
2. Bayes BJ. Prone infants and SIDS. N Engl J Med 1974:290:693-4. [ Links ]
3. Mitchell EA. Sleeping position of infants and the sudden infant death syndrome. Acta Paediatr Suppl 1993;389:26-30. [ Links ]
4. Amemiya F, Vos JE, PrechtJ HE. Effects of prone and supine position on heart rate, respiratory rate and motor activity in fullterm newborn infants. Brain Dev 1991;13:148-54.
5. Adams JA, ZabaJeta IA, Sackner MA. Comparison of supine and prone noninvasive measurements ofbreathing patterns in fullterm newborns. Pediatr Pulmonol 1994; 18:8-12. [ Links ]
6. Wagaman MJ, Shutack JG, Moomjian AS, Schwartz JG, Shaffer TH, Fox WW. lmproved oxygenation and lung compliance with prone positioning of neonates. J Pediatr 1979;94:787-91. [ Links ]
7. Lioy J, Manginello FP.Acornparison of prone and supine positioning in the immediate postextubation period of neonates. J Pediatr 1988;112:982-4.
8. Maynard V,Bignall S, Kitchen S. The effect of positioning on the stability of oxygenation and respiratory synchrony in nonventilated pre-term infants. J CJin Nurs 1999;8:479-81. [ Links ]
9. Dimitriou G, Greenough A, Pink L, McGbee A, Hickey A, Rafferty GE. Effect of posture on oxygenation and respiratory muscle strength in convalescents infants. Arch Dis Child Fetal Neonatal 2002;86: 147-50. [ Links ]
10. Ballard JL, Khoury JC, Wedig K, Wang L, Eilers-Walsman BL, Lipp R. New Ballard Score, expanded to include extremely premature infants. J Pediatr 1991;119:417-22. [ Links ]
11. Khan N, Brown A, Venkataraman ST. Predictors of extubation success and failure in mechanically ventilated infants and children. Crit Care Med 1996;24: 1568-79. [ Links ]
12. Berquó ES, Souza lMP, Gotlieb SLD. Bioestarística. 2ª ed. Sao Paulo: Pedagógica e Universitária; 1981.
13. Rugolo LMSS. Assisténcia ao recém-nascido de muito baixo peso. In: UNESP. Departamento de Pediatria da Faculdade de Medicina de Botucatu. Condutas em Pediatria. 4ª ed. Rio de laneiro: EPUB; 1999.p.146-9.
14. Chatila W, lacob S, Guaglionone D, Manthous CA. The unassisted respiratory rate-tidal volume ratio accurately predicts weaning outcome. Am J Med 1996;101:61-7.
15. Wolfson MR, Greenspan JS, Deoras KS, Allen JL, Shaffer TH. Effect of position on the mechanical interaction between the rib cage and abdomen in preterm infants. J Appl Physiol 1992;72: 1032-8. [ Links ]
16. Mendonza JC, Roberts JL, Cook LN. Postural effects on pulmonary function and heart rate of preterm infants with lung disease. J Pediatr 1991;118:445-8. [ Links ]
17. Sahni R, Schulze KF, Kashyap S, Ohira-Kist K, Myers MM, Fifer WP. Body position, sleep states, and cardiorespiratory activity in developing low birth weight infants. Early Hum Dev 1999;54: 197-206. [ Links ]
18. Brackbill Y, Douthitt TC, West H. Psychophysiologie effects in the neonate of prone versus supine placement. J Pediatr 1973; 82:82-4. [ Links ]
19. Quinn W, Sandifer L, Goldsmith JP. Pulmonary careo. En: Goldsmith JP, Karotkin EH. Assisted ventilation of the neonate. 3ª ed. Filadélfia: WB Saunders Company; 1996. p.101-23. [ Links ]
20. Page N, Giehl M, Luke S. Intubation complications in the critically ill child. Am AACN Clin Issues 1998;9:25-35. [ Links ]
21. Rugolo LMSS. CPAP. In: Alves Filho N, Trindade Filho O, editores. Clínica de Perinatologia. V. 1. Rio de Janeiro: Medsi ; 2001. p.73-81. [ Links ]
22. Kavvadia V, Greenough A, Dimitriou G. Prediction of extubation failure in preterm neonates. Eur J Pediatr 2000;159:227-31. [ Links ]
23. Mador MJ. Weaning from mechanical ventilation: What have we learned and what do we still need to know?. Chest 1998;114:672-4. [ Links ]
24. Meade M, Guyatt G, Cook D, Griffith L, Sinuff T, Kergl C, et-al. Predicting success in weaning from mechanical ventilation. Chest 2001 ;120:400S-24S. [ Links ]
25. Chatte G, Sab JM, Dubois JM, Sirodot M, Gaussorgues P, Robert D. Prone position in mechanically venti1ated patients with severe acute respiratory failure. Arn J Respir Crit Care Med 1997; 155:473-8.
26. Curley MA, Thompson JE, Arnold JM. The effects of early and repeated prone positioning in pediatric patients with acute lung injury. Chest 2000; 118:156-63. [ Links ]
Correspondencia
Enderece para correspondencia:
Dra. Letícia Cláudia de Oliveira Antunes
UTI Neonatal do Hospital das Clínicas da Faculdade de Medicina de Botucatu-UNESP ]]>
Rua Dr. José Adriano Marrey Júnior, 622
CEP 18603-610 Botucatu. SP
E-mail: letantunes@hotmail.com.br