Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Revista Latinoamericana de Desarrollo Económico
versión On-line ISSN 2074-4706
rlde n.35 La Paz 2021
Life and Death During the First Year of the COVID-19 Pandemic: An analysis of cross-country differences in changes in quantity and quality of life
Vida y muerte durante el primer año de la pandemia COVID-19: un análisis de las diferencias entre países en los cambios en la cantidad y la calidad de vida
Lykke E. Andersen *, Alejandra Gonzáles Rocabado **
Abstract***
This study carries out a cross-country analysis of changes in quantity and quality of life during the first year of the COVID-19 pandemic for 124 countries. Changes in the quantity of life are measured as life years lost to COVID-19, including excess deaths not officially reported as COVID-19 deaths. Changes in quality of life are proxied by the average change in daily mobility, compared to a pre-COVID baseline. We find a significant negative correlation between the two, meaning that the countries with the biggest reductions in mobility are also the countries with the biggest losses of life years. We calculate that about 48 million life years were lost during the first year of the pandemic, corresponding to 0.018% of all expected life years. For comparison, at least double the amount of life years are lost every year due to children dying of diarrhea. About 28 million life years are created every day from babies being born, so the first year of the pandemic set us back less than two days in terms of quantity of life. The setbacks in terms of quality of life are several orders of magnitude larger. Some countries have suffered close to a 50% reduction in mobility sustained over 12 months, with devastating effects on many aspects of quality of life. We estimate that 1.2 billion quality life years were lost due to mobility reductions, which is 25 times as many as life years lost due to COVID-19 related deaths during the first year of the pandemic.
Keywords: COVID-19; pandemic; life years; mobility; quality of life.
Resumen
Este estudio realiza un análisis comparativo de los cambios en la cantidad y la calidad de vida durante el primer año de la pandemia COVID-19 para 124 países. Los cambios en la cantidad de vida se miden como años de vida perdidos por COVID-19, incluido el exceso de muertes no reportadas oficialmente como muertes por COVID-19. Los cambios en la calidad de vida están representados por el cambio promedio en la movilidad diaria, en comparación con una línea base anterior al COVID-19. Encontramos una correlación negativa significativa entre los dos, lo que significa que los países con mayores reducciones de movilidad son también los países con mayores pérdidas de años de vida. Calculamos que se perdieron alrededor de 48 millones de años de vida durante el primer año de la pandemia, lo que corresponde al 0.018% de todos los años de vida esperados. A modo de comparación, se pierden al menos dos veces más años de vida cada año debido a la mortalidad de niños por diarrea. Todos los días se generan alrededor de 28 millones de años de vida por el nacimiento de bebés, por lo que el primer año de la pandemia nos retrasó menos de dos días en términos de cantidad de vida. Los contratiempos en términos de calidad de vida son de varios órdenes de mayor magnitud. Algunos países han sufrido una reducción de alrededor del 50% en la movilidad durante los últimos doce meses, con efectos devastadores en muchos aspectos de la calidad de vida. Estimamos que 1,200 millones de años de calidad de vida han sido perdidos por las reducciones en movilidad, lo cual es 25 veces más que la cantidad de años perdidos por muertes de COVID-19 en el primer año de la pandemia.
Palabras clave: COVID-19; pandemia; años de vida; movilidad; calidad de vida.
Classification/Clasificación JEL: H12,I14,I18,I38.
The numbers have no way of speaking for themselves.
We speak for them, we imbue them with meaning
Nate Silver
1. Introduction and motivation
The COVID-19 pandemic, caused by the SARS-CoV-2 virus, has confronted people and governments across the globe with tough life-and-death decisions: Should grandma be allowed to hug her grandchildren? Should children be allowed to go to school? Should colleagues be allowed to enjoy a beer together Friday afternoon? Should teenagers be allowed to go to the beach? Would it be OK to go for a run in the park Sunday morning without a face mask?
We are already more than one year into the pandemic, but many governments are still not sure what the correct answers to those questions are. Indeed, in many countries the answers may change from one week to the next, causing major uncertainty for businesses, students, travelers, bureaucrats, and the population in general. The best answers also vary considerably from person to person, as some groups are more vulnerable to the virus, while other groups are more vulnerable to the restrictions implemented to control the virus.
In this paper, we will evaluate the experiences during the first year of the pandemic (from 11 March 2019 to 11 March 2021) from across the world, in order to extract some recommendations for the remainder of the pandemic, as we still have quite some way to go before the pandemic is over. Since all aspects of life are affected by the pandemic, including health, education, work, investment, pleasure, travel, inequality, poverty, violence, democracy, freedom, and mobility, it is necessary to employ a broad perspective covering all these dimensions.
Viruses outnumber people on the planet by approximately 143,000,000,000,000,000,000 to 11, so there is no way to avoid being exposed to viruses. In addition, the only way that viruses can replicate themselves is to enter the cells of another organism, and convince the reproductive apparatus of that cell to reproduce the virus's genetic structure instead of its own. Thus, viruses depend completely on their hosts to survive, and have no interest in killing them. Most viruses have a favorite host, and do not harm that host, because that would be self-defeating.
However, once in a while, random mutations occur that allow the virus to jump to another species, which is not used to live with that virus. Given the vast number of viruses involved, and their rapid rates of multiplication, this happens quite frequently. To deal with that, humans, and indeed all other living organisms, have had to develop defense mechanisms. This defense mechanism is our immune system, which, through millions of years of evolution together with millions of different virus species, has developed several layers of defense against the constant onslaught of potential pathogens. The human innate immune system includes barrier tissues with antimicrobial chemicals, white blood cells trained to recognize potential pathogens, macrophages that ingest and kill viruses, natural killer cells that destroy infected cells, cytokines and chemokines that send signals to other innate immune cells about ongoing problems, and much more. If the innate immune system is not enough, we have a second layer of defense called the adaptive immune system, which deals with particularly tough threats. This adaptive immune system includes cytotoxic T cells trained to kill what looks like a pathogen, B cells which produce antibodies that bind to pathogens in order to neutralize them, and memory B cells which remember how to deal with a specific threat if it should encounter it again in the future2. The adaptive immune system can be activated either by direct infection or by vaccination, which is designed to mimic infection, and prompt the immune system to produce antibodies.
Our bodies usually manage all this without us having to think about it consciously. However, once in a while, a particularly nasty virus mutation will appear, and if we don't identify it quickly and eradicate it early, it may cause a worldwide pandemic with high excess mortality rates.
Due to the huge numbers of viruses involved, these dangerous mutations happen regularly, with almost mathematical precision. However, due to increased global travel, increased population densities, and increased industrial animal production, the risk of a dangerous pandemic has increased steadily over the past century, and this trend will likely continue and intensify. There has been no shortage ofwarnings about these risks, both from scientists and science fiction, and the global community has been developing systems to deal with particularly nasty mutations.
While we have become increasingly susceptible to a dangerous virus mutation, we have also become much better at dealing with the threat, as the scientific understanding of viruses has increased tremendously. One hundred years ago, nobody understood even the basics of the Spanish Flu. In 2020 scientists managed to sequence the whole DNA of the SARS-CoV-2 virus within a few weeks of discovering it, and made it publicly available in the GenBank database (accession number MN908947) on 10 January 2020. This allowed other researchers to immediately start developing test kits to detect cases in other countries (ECDC, 2020). It also allowed research teams around the world to quickly start developing potential vaccines. Currently, more than a hundred vaccine candidates are being tested (Gavi, 2020). Impressively, several vaccines passed rigorous safety and efficacy trials and got approved for massive vaccination roll-outs within one year of detecting the new virus -a feat never before accomplished. The COVID-19 vaccine race can now be followed in real time at sites such as Our World in Data: https://ourworldindata.org/covid-vaccinations.
While some countries were prepared for a pandemic (mainly due to practice from previous scary viruses), and more or less followed previously devised plans and strategies to manage the new virus, many others were caught off guard and had to improvise. It is still too early to make final judgements concerning the management of the COVID-19 pandemic, but in this paper, we take stock of the outcomes of the decisions taken during the first year of the pandemic in 124 countries across the world. We urgently need to learn from both good and bad experiences in order to get through the rest of the pandemic with the least damage possible.
The differences between countries are astonishingly large, especially in terms of mortality rates, which vary more than a hundred-fold so far. Some of these differences may be due to structural differences (such as differences in the age composition of the population, obesity rates, population density, quality of the health care system, etc.); some may be due to differences in behavior (such as working from home, wearing masks, using hand sanitizers, or maintaining physical distancing); and some may be due to differences in the timing of the pandemic, in the amount of testing, and in how cases and deaths are counted and reported.
Surprisingly, there can be very large differences in health outcomes even within the same country. For example, Figure 1 shows excess mortality in Italy by week and by region, comparing the first 10 months of 2020 to average all-cause deaths per week during the previous 10 years. Lombardy, a region in northern Italy that includes the metropolitan area of Milan, saw more than 27 thousand excess deaths between February and October, implying that at the peak of the outbreak the region saw 3 to 4 times the normal number of deaths. In contrast, the Lazio region, which includes Rome in the central part of Italy, saw 136 fewer deaths than normal during the first 10 months of 2020.

There have also been very large differences in the response to the pandemic. Some countries managed to get systems of testing and contact tracing up and running very quickly which allowed them to identify and isolate infected individuals and to squash every outbreak to avoid the virus spreading in the community. On the 13th of January 2020, Thailand became the first country to detect a COVID-19 case outside China. The next 14 cases detected in Thailand were all in travelers arriving from China, but by 31 January the first non-imported, locally transmitted case was detected. By the end of March, 60 of Thailand's 77 provinces had reported cases and the epidemic was widespread, but Rapid Response Teams quickly managed confirmed cases by isolating and treating them, and tracing and quarantining their contacts. All cases were isolated in facilities rather than in their homes. By the end of April, local transmission had been controlled across the country (World Health Organization, 2020a). Currently, there are few restrictions on activity or movement within Thailand though borders remain closed to most travelers, which is obviously a major problem for a country with a world famous tourism industry.
Other countries realized too late that the SARS-CoV-2 virus was already circulating widely and asymptomatically, but did not have the testing capacity to identify who was infected and who was not, so they instead went for crude lockdowns, hoping that this would prevent the virus from being able to spread. As we will see in this paper, this clearly did not work, even in countries with some of the toughest lockdowns in the world, such as Peru and Bolivia.
A few countries (most notably Sweden) figured out early on that this virus was going to be with us for a long time, and that we needed to implement measures that could be sustained over time. The Swedish strategy relies to a large extent on the wise decisions of the population, rather than compulsory measures and forced school and business closures. Sweden has been heavily criticized for its light-touch approach, but for research purposes, it is great to have a benchmark case to compare with.
The objective of this paper is to quantify the outcomes of the decisions and behaviors during the first year of the pandemic in 124 countries in two main dimensions: Life and Death. It is still too early to make final judgements, but we urgently need to learn from both good and bad experiences.
The remainder of the paper is organized as follows. Section 2 reviews the key literature that the paper is building upon. Section 3 describes the methodology and the data used. Section 4 shows the cross-country results. Section 5 attempts to put COVID-19 into perspective by calculating the magnitude of the setbacks in different dimensions of life and death. Finally, section 6 provides a summary as well as policy recommendations.
2. Key literature
During the early months of the COVID-19 pandemic, there was still very limited data to learn from, so many researchers turned to the 1918 Spanish Flu for lessons to be learned. Beach, Clay and Saavedra (2020) provide an excellent overview of the main outcomes of the Spanish Flu. They report that roughly 50 million people died from influenza between 1918 and 1920, mostly in India and China. In total, 26-36 million deaths occurred in Asia, while Africa and Europe each saw about 2.5 million deaths, and the Americas only about 1.5 million. This is almost the opposite geographical pattern as the COVID-19 pandemic, which so far has seen the highest death rates in North America, South America and Europe, while Africa, Asia and Oceania have seen deaths per million inhabitants at least an order of magnitude lower (Dong, Du and Gardner, 2020).
Beach, Clay and Saavedra (2020) considered that a leading explanation for differences in death rates during the 1918 pandemic was income levels. Murray et al. (2006) regressed country level excess mortality rates on per capita income levels in 1918 and found that income was negatively and significantly related to death rates. A 10% increase in income was associated with a 9-10% decrease in mortality. They predicted that if a similar influenza pandemic were to occur in 2004, 96% of deaths would occur in developing countries. Surprisingly, we have observed the opposite pattern with COVID-19.
Another major difference between the 1918 flu pandemic and the 2019 coronavirus pandemic highlighted by Beach, Clay and Saavedra (2020) is that the former killed many prime-aged workers, whereas COVID-19 kills mainly old people. The different age profiles of risk alone would imply completely different impacts on the economy and society, which should make us further hesitant to transfer the lessons from the 1918 pandemic to our current predicament. Not to mention that our knowledge about viruses, our capacity to develop vaccines, and our ability to work online have changed drastically since 1918.
While human society has changed dramatically over the last 100 years, viruses tend to work the same way as they have for millions of years. Thus, we can learn a lot from observing the biological evolution of past pandemics. For example, it is worth pointing out that the 1918 influenza pandemic continues even to the present day, with tens of thousands of people being killed every year by new variants that have all evolved from the original H1N1 influenza virus which caused the 1918 pandemic (Taubenberger, Kash and Morens, 2019). Fortunately, subsequent strains have been much less lethal than the original (Taubenberger and Morens, 2006).
Like several other recent papers on this and previous pandemics, our paper is descriptive-comparative. We try to quantify how countries have been performing in both the life and death dimensions during the pandemic, and compare outcomes across countries in order to learn from good and bad experiences.
The paper is most directly related to the World Bank study by Decerf, Ferreira, Mahler and Sterck (2020) which estimates years of life lost (LY) and additional years spent in poverty (PY) due to the pandemic until early June 2020. The authors find that the ratio of PYs to LYs is very large, especially in poorer countries, implying that we certainly have to include the impacts on peoples livelihoods as well as on their lives.
To estimate years of life lost, LY, the authors use age-specific mortality information, and assume that LY is equal to the residual life-expectancy at the age of death, as computed from the country's pre-pandemic age-specific mortality rates, which were obtained from the Global Burden of Disease Database (Dicker et al., 2018).
We will use a similar calculation of life years lost, but instead of using only reported COVID-19 deaths, we will include excess deaths that have not been reported as COVID-19. Excess mortality is a far more accurate measure of health impacts of the pandemic, especially in countries where testing has been highly restricted, or where there have been many collateral deaths due to overwhelmed hospital systems, lockdowns, or unemployment. The European Mortality Monitoring Initiative, EUROMOMO3, is a model for this kind of monitoring, and it has inspired several similar initiatives during this pandemic. For example, the New York Times now maintains a database on excess mortality4, as does The Economist5 and Financial Times6. The data used to be scattered, but Ariel Karlinsky and Dmitry Kobak have made a huge effort to gather weekly, monthly, or quarterly all-cause mortality data from as many countries as possible, and have made this data openly available as the regularly-updated World Mortality Database (Karlinsky and Kobak, 2021), which we use in this paper.
To estimate years spent in poverty (PY), Decerf et al. (2020) use information about each country's income distribution, each country's poverty line7, and the changes in economic growth estimates between January and June 2020, according to the World Bank's Global Economic Prospects (GEP) (World Bank, 2020a). Their method requires quite a lot of assumptions, including the conservative assumption that the additional poverty induced by COVID-19 will only last for one year. It is still far too early to know if these assumptions are reasonable, so in this paper we will offer an alternative way of measuring the livelihoods dimension of the analysis.
While the increase in income poverty is clearly one of the most dramatic effects of this pandemic, the deprivations suffered go far beyond the lack of income. As suggested by the introductory paragraph of this paper, the pandemic has prevented grandparents from spending time with their grandchildren, has made it impossible for children to go to school, has made it illegal for colleagues to enjoy a beer Friday afternoon, and in many places people have not even been allowed to enjoy nature.
A potentially useful way to summarize all these diverse effects is to measure how the pandemic has affected our interactions with other people. For that purpose, the Google Community Mobility Reports (Google, 2020), based on the movements of our cell-phones, are extremely useful. These reports show how the number of visits and the length of stay at different types of places (retail and recreation; grocery and pharmacy; parks; transit stations; workplaces; and residential) have changed during the pandemic compared to a pre-pandemic baseline (3 January to 6 February 2020). The data is calculated for most countries in the world, and even at sub-national levels for some of them. Given that there are by now more cellphone subscriptions than people on the planet8, this data is likely to be reasonably representative for the whole population in most countries. Unfortunately, data is lacking for some big countries, like China and Ethiopia. One additional concern is that the averages may hide systematic differences by age and gender. Caselli et al. (2021) obtained a unique data set from Vodafone for Italy, Portugal, and Spain, and found that lockdowns had a larger impact on the mobility of women and younger cohorts. This is important to bear in mind when interpreting our results.
Several other studies have used the Google mobility data to analyze how countries have performed during the pandemic. The Sustainable Development Report 2020, prepared by Sachs et al. (2020), is probably one of the first worldwide studies that use Google Mobility Data to assess how well countries performed during the early months of the pandemic. They constructed a COVID Index of Epidemic Control (CIEC) which summarizes each country's performance over three dimensions:
Cumulative COVID-19 mortality rate, per million inhabitants, as of 12 May 2020.
The average Effective Reproduction Rate (ERR)9 during 4 March to 12 May 2020.
Epidemic Control Efficiency (ECE), which is calculated as the difference between the proportionate reduction in ERR and the proportionate reduction in mobility10, from 4 March to 12 May 2020.
According to Sachs et al. (2020), reductions in mobility are a very costly and inefficient way of reducing the ERR and thus the mortality rate, which is why high reductions in mobility lower the performance of the index. During their period of analysis, South Korea experienced a 10% reduction in mobility, while maintaining a low mortality rate of 5 COVID-19 deaths per million inhabitants, which is considered highly efficient. In contrast, Spain experienced a 60% reduction in mobility while reaching 575 COVID deaths per million inhabitants by 12 May 2020, which is extremely inefficient.
Bargain and Ulugbek (2020) analyze the Google mobility data in more detail to assess how changes in work mobility depend on the level of poverty. They show that across 241 regions of 9 countries from Latin America and Africa, the decline in work mobility after lockdown is significantly lower in regions with higher poverty rates, since people simply cannot afford to stay at home. They also estimate that poverty rates one standard-deviation above the mean regional poverty are associated with 11 % more cases after a month and a half.
3. Methodology and data
The SARS-CoV-2 virus, despite having a relatively low infection fatality rate (Ioannidis, 2020), has had more dramatic impacts on all aspects of life, across the entire world, than any other virus during the last 100 years. Thus, when analyzing how well countries have managed the pandemic so far, we need to include more than just the number of COVID-19 infections and deaths, which every country on the planet seems to report daily.
Assessing all impacts simultaneously for all countries is obviously empirically challenging. In this paper we will assess two major groups of effects: i) Effects on death and ii) effects on life. That leaves out some major effects on governments and public finances, but obtaining data to assess that will require more time.
3.1. Measuring the death dimension
The most commonly used way of gauging the deadly impacts ofCOVID-19 is accumulated deaths per million inhabitants. This metric is updated daily by several sites, such as Worldometer11 and Our World in Data12. The results so far show astonishing differences between countries, ranging from less than 10 per million (e.g. Taiwan, Tanzania, Thailand, Niger, New Zealand, Myanmar, Mongolia, Uganda, among others) to more than 1,000 per million (e.g. USA, Brazil, UK, Italy, Mexico, France, Colombia, Argentina and Peru, just to mentions some of the biggest).
This data, however, suffers from serious problems of under-reporting in many countries where COVID-19 testing was severely limited during most of the early phases of the pandemic, or where reporting guidelines implied that only COVID-19 deaths in hospitals were counted. In other countries, the lack of testing may have led to over-reporting, since any death with COVID-like symptoms or in persons who had previously tested positive for COVID-19 were included.
This problem of under- and over-reporting has been widely acknowledged, and, as mentioned above, several institutions have implemented major efforts to monitor excess mortality. In this paper we use excess mortality data from the World Mortality Database, which covers 71 of our countries (Karlinsky and Kobak, 2021). Some countries report deaths every week, others every month, and some only every quarter. Only one country (Peru) was completely up to date with excess deaths until our cut-off date (11 March 2021), so for the rest we add official COVID-19 deaths between the last date of excess death reporting and 11 March 2021 to get the most accurate number possible of excess deaths between 1 January 2020 and 11 March 2021. Annex provides details.
One additional consideration, that has to be taken into account, is the age of the people who died prematurely. A person dying at 23 years of age will lose many more expected life years than a person dying at 93. It is well-known that care homes, nursing homes and other assisted living facilities have been particularly hard hit by COVID-19 in many countries. But care homes tend to be places where people are spending the last few months or years of their life, because they have become so old and frail that they are no longer able to take care of themselves.
In order to take into account differences in the age structure of COVID-19 associated deaths, we apply the methodology of Decerf et al. (2020). Combining information on the age pyramid in each country, the residual life expectancy by age in each country, and inferred COVID-19 deaths by age in each country, they estimate how many life years are lost, on average, for each COVID-19 death in each country. The authors have kindly shared their calculations with us, and we simply use their estimates of life years lost per COVID-19 death, which range from a minimum of 8.1 years in Latvia to a maximum of 20.0 years in Iraq. These estimates are in line with those of Pifarré-i-Arolas et al. (2021) which study 81 countries in more detail and arrive at an average of 16 life years lost per COVID-19 death. The latter study differentiated lost deaths by gender, and found that men had lost 45% more life years than women, both because men are more likely to die from COVID-19 than women, and because they die at a younger age. We do not distinguish between men and women in our calculations, but these gender differences are important to bear in mind when interpreting the results.
We express the total number of life years lost as a percentage of the total remaining life years of the population pre-COVID-19 and call this variable DDeath. Given that even in the worst hit countries less than half a percent of the population has died due to COVID-19, and given that most of those who died were already quite old, the percentage of lost life years is so far below 0.2% for all countries.
3.2. Measuring the life dimension
To measure changes in the life dimension, we use daily mobility data from the Google (2020) Community Mobility Reports, which aggregate anonymized data from the location history of mobile phones in most countries of the world. These reports were specifically created to provide information to help monitor and manage the pandemic. They record percent changes, compared to a baseline, in the number of visits or length of stay at six different types of location:
1. Retail and Recreation: Restaurants, cafes, shopping centers, theme parks, museums, libraries, and movie theaters.
2. Grocery and Pharmacy: Grocery markets, food warehouses, farmers' markets, specialty food shops, drug stores, and pharmacies.
3. Parks: Local parks, national parks, public beaches, marinas, dog parks, plazas, and public gardens.
4. Transit Stations: Public transport hubs such as subway, bus, and train stations.
5. Workplaces: Places of work.
6. Residential: Places of residence.
The baseline is calculated during the five-week period from 3 January to 6 February 2020, as the median value for the corresponding day of the week.
For the first five categories of location, the reports show the percentage change in the number of visits, whereas, for the residential category, they show the change in length of stay.
In order to create a summary measure of how the pandemic has impacted the quality of our lives during the first year of the pandemic, we calculate a DLife index which is the simple average of the daily changes in visits to the first five categories of locations over the period of analysis, compared to the baseline.
We have given the same weights to each of the five categories of locations, although in reality people probably did not visit each of these areas with the same frequency in the baseline period. However, to protect privacy, Google (2020) does not report absolute values, only percent change, so we don't have the necessary information to establish differentiated weights.
3.3. Period of analysis
The period of analysis is the first 12 months since the World Health Organization officially declared COVID-19 a pandemic, that is from 11 March 2020 to 11 March 2021.
The virus spread quickly across the world, and most countries failed to suppress the outbreak, which means that significant spread occurred, especially in densely populated areas. Seroprevalence studies indicate that in New York city 22.7% had been infected by March 2020 (Rosenberg et al., 2020); in Oise, France 25.9% had been infected by late March (Fontanet et al., 2020); in the Guilan province of northern Iran about 33% of the population showed antibodies by April (Shakiba et al., 2020); in Rio de Janeiro 3-4% of the population showed antibodies by late April (Amorim Filho et al., 2020); in Kenya, the share was about 5% by late May (Uyoga et al., 2020); in Manaus, Brazil it reached 52% by June (Buss et al., 2020); in urban Pakistan, it reached 17.5% by early July (Javed et al., 2020); in Qatar, it reached 30.4% in early July (Abu Raddad et al., 2020); in Mumbai slums, it reached about 58% by early July (Malani et al., 2020); and it was close to 50% in Tokyo by late August (Hibino et al., 2020).
Still, the pandemic is by no means over, and it is too early to make final judgements, but guidance to countries is urgently needed, so we have to make do with preliminary analyses for now.
3.4. Countries included
Our analysis requires enormous amounts of data, so only countries that collaborate and contribute to the various global efforts of generating reliable and comparable data are included. Specifically, we only take into account countries that simultaneously are included in the Google Mobility data initiative, and provide sufficient data to be incorporated in the Sustainable Development Report 2020.
We have grouped the 124 countries with complete data in 4 main groups defined by location, and they are listed in Table 1.
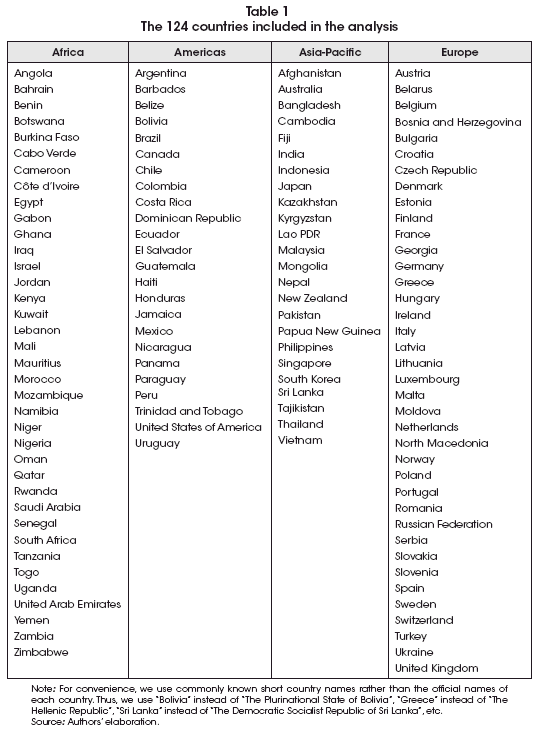
These countries comprise the majority of the Worlds population (approximately 5.6 billion people), but they also exclude some really large countries. For example, China and Ethiopia were not taken into account because they are not included in the Google Mobility data set.
These 124 countries accounted for 95.9% of all official COVID-19 deaths in the World during the first year of the pandemic.
4. Cross-country results
4.1. Life and Death diagrams
This section presents the main cross country results in a series of Life and Death diagrams. The horizontal axis of each graph represents changes in the quality of life, DLife, as measured by the average change in daily mobility during the period 12 March 2020 to 11 March 2021. The vertical axis represents changes in the quantity of life, measured in different ways, all from 1 January 2020 to 11 March 2021.
Figure 2 shows official COVID-19 deaths per million inhabitants against average changes in daily mobility. Due to the widespread quarantines and precautionary actions of the populations, few countries have seen positive changes inmobility compared to the baseline, but there are a few exceptions worth mentioning, notably Denmark and Sweden. These positive changes are mainly due to the baseline period being mid-winter for the northern hemisphere, so it is natural to see an increase in visits to parks compared to January. In Denmark and Sweden, we do indeed observe big increases in visits to parks compared to baseline (101% and 84%, respectively), while in both countries there are significant reductions of around 30% to transit stations and workplaces. It is worth noting, though, that the UK has the same climate as Denmark, and in the UK the increase in visits to parks was only 22% compared to baseline, far from the 101 % increase seen in Denmark.
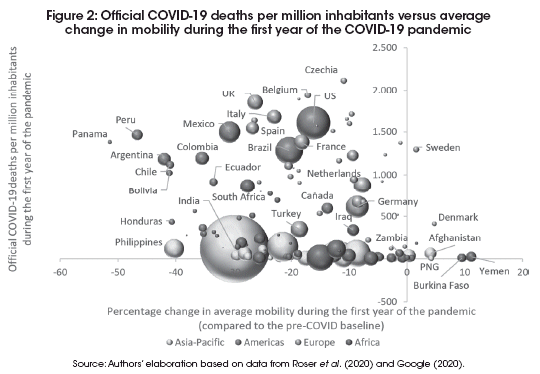
The correlation between the two indicators in Figure 2 is -0.19, implying a very weak negative relationship between changes in mobility and COVID-19 death rates. In general, the countries of Asia and Africa experienced low death rates, while the countries of the Americas and Europe have experienced relatively high death rates.
Basu, Basu and Tapia (2020) argue that it is important to evaluate countries within their own region, as there are striking differences in death rates between regions, likely due to the history of past diseases. For the Africa group the correlation is -0.41, for Europe it is -0.33, for the Americas -0.28, and for Asia -0.10. In no region do we see a positive relationship suggesting that mobility restrictions help reduce COVID-19 death rates, at least not in the medium term of a year. They may work for a little while, but unless the measure successfully eradicates the virus, and the country maintains its borders closed until the pandemic is over, then lockdowns at most serve to spread the deaths out over time.
However, Figure 2 only includes officially reported COVID-19 deaths, and the countries with very high death rates also had very limited testing capacity, at least during the first wave, so not all COVID-19 deaths got reported. A more accurate impression is provided by the number of excess deaths registered during the period of analysis. Figure 3 shows excess deaths per million inhabitants versus average change in mobility. Taking into account excess deaths changes the scale of the vertical axis, but otherwise does not change the main picture. When taking into account excess deaths rather than officially reported COVID-19 deaths, the death rate per million for Peru increases from 1,466 to 4,442, which means that almost 0.5% of the entire population died during the first year of the pandemic. And this despite having observed one of the strictest lockdowns in the world throughout the year, as evidenced by a reduction in average daily mobility of almost 50% sustained over the entire year.
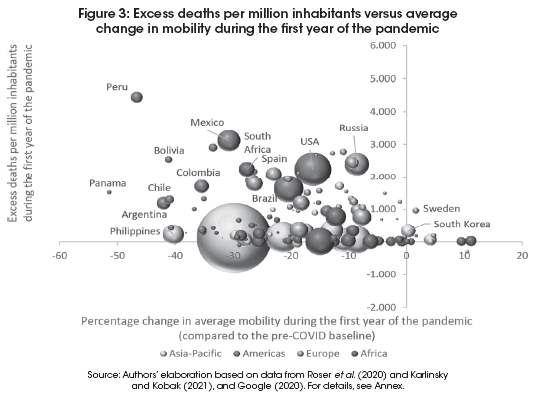
The correlation between the two indicators in Figure 3 is -0.26, suggesting that the countries that have seen the biggest reductions in mobility have also seen the highest excess mortality rates, although the relationship is not very strong.
Since the death of a young person implies many more lost life years than the death of an older person, we can further refine the analysis by calculating the total number of life years lost due to COVID-19, and compare this to the expected remaining life years of the population in each country.
In total, the world lost approximately 48 million life years to COVID-19 during the first year of the pandemic. Figure 4 shows the 30 countries that lost most life years. The 30 countries included in Figure 4 account for about 90% of all excess deaths in our 124 countries during the first year of the pandemic13.
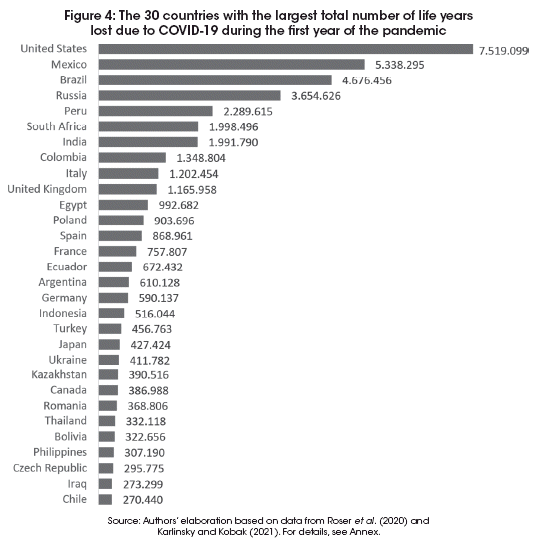
The United States heads the list. With an estimated 736,123 excess death causing an average loss of 10.2 years of life per death, the total loss during the first year of the pandemic is about 7.5 million life years.
The remaining life years for the entire pre-COVID population of the United States was about 14 billion, though, so in percentage terms, only 0.054% of total life years were lost due to COVID-19 during the first year of the pandemic. Figure 5 plots the percentage loss of life years for each country against the percentage loss in mobility.
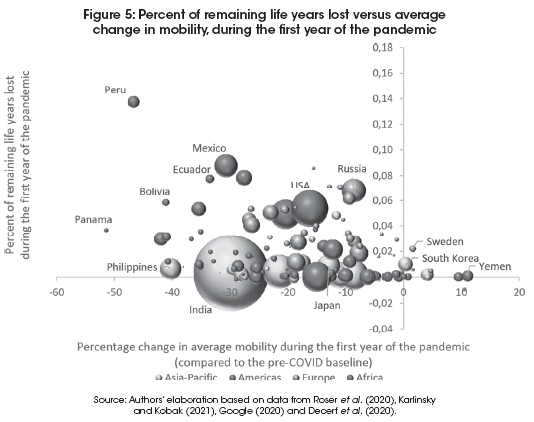
Peru is still the most extreme example, having lost 0.137% of total life years due to COVID-19 during the first year of the pandemic, while during the same time period average daily mobility was reduced by almost 50%. At the other extreme, we find a variety of countries with an increase in mobility compared to the baseline (Sweden and Denmark in Europe, South Korea, Mongolia, Afghanistan and PNG in the Asian group, and Benin, Botswana, Burkina Faso, Togo and Yemen in the Africa group). All of these with total loss of life years less than 0.022%.
The correlation between the two indicators in Figure 5 is -0.28, suggesting that there is definitely no trade-off between protecting economic/human activity and protecting lives. The countries that have fared badly in one dimension have generally also fared badly in the other.
The negative relationship is even stronger when calculated by region, rather than for all countries together. For the Africa group the correlation is -0.43, for Europe it is -0.30, for the Americas -0.27, and for Asia -0.11. In no region do we see a positive relationship suggesting that mobility restrictions help reduce death rates in the medium term.
4.2. Total welfare impacts of the pandemic
In the previous sub-section, we graphed the Life and Death dimensions against each other, but if we are willing to make a simple assumption, we can actually add the two dimensions together and arrive at an estimate of total welfare loss for each country during the first year of the pandemic.
The assumption we need to make is that a 100% reduction in mobility for a year is equal to a lost year of life. Basically, imagine a year in solitary confinement without interaction with friends, family, colleagues or even strangers. You can't work, you can't go shopping, and you can't go for a walk around the block to get some sun, much less for a hike in nature. The only thing you are allowed to do is to use your cellphone to access the Internet, but you will probably have to be quite selective about that, since your monthly Internet allowance is limited. If you are very lucky, you have a computer with unlimited Internet access, in which case the loss may feel less severe. You may also have your spouse and kids with you, which may or may not make you feel better.
If we are willing, for the moment, to make that assumption, then we can calculate the amount of Quality Life Years (QLY) lost in each country by multiplying the percentage change in mobility with the size of the population. So, for example, a country with a million inhabitants who on average reduced their mobility by 20% during the first year of the pandemic, would have lost 200,000 QLY. We can then add these to the Life Years (LY) lost due to excess deaths caused by the pandemic to obtain the Total Years (TY) lost. Finally, we can divide that by the population size and multiply by the number of days in the year, in order to get Quality Days lost per person (QDpc) during the first year of the pandemic.
Figure 6 plots the results against the Sustainable Development Index of 2020, as calculated by Sachs et al. (2020). There is a clear hump-shaped relationship indicating that the least developed countries and the most developed countries saw the lowest total losses in welfare during the first year of the pandemic, while countries with medium levels of sustainable development saw the highest losses. Panama and Peru both lost almost 200 Quality Days per person during the first year of the pandemic. The weighted average for the 124 countries in our sample was 77 QDpc.
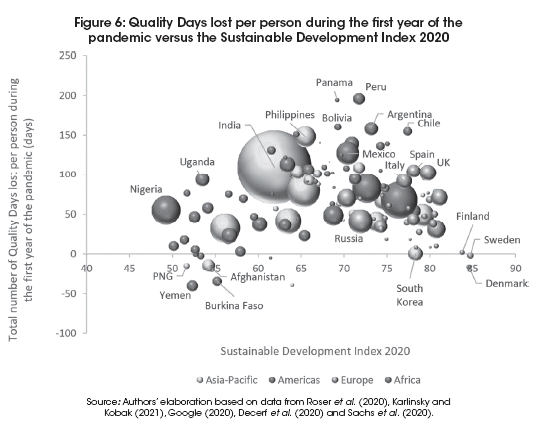
On average, the world lost 25 times more quality years of life due to mobility restrictions than due to COVID-19 related deaths, but for some countries this ratio was much higher. For the Asia group the ratio was a whopping 131, implying that for each year of life lost to COVID-19, 131 quality years of life were lost due to mobility restrictions. This result is mainly driven by the big countries with strong restrictions, but low death rates, such as the Philippines and India. For details for each country, please see Annex.
For Europe and the Americas, the ratio was lower, both at 10, due to the much higher death rates in these regions. This is still a high ratio, however, if one considers a year with 100% mobility reduction to be as bad as a year of life lost. Perhaps in highly developed countries with good Internet connections, young people might be willing to spend several years locked in a room with a computer, getting fed without having to work or study, in order to give their grandfather an extra year of life. But that seems to be a rather dystopian situation, and it doesn't make much sense from a public policy point of view, as the future of our societies depends on our current investments in the human capital accumulation of the young.
Only 13 countries out of the 124 countries analyzed in this paper have achieved a certain balance between life years lost to COVID-19 and quality years of life lost to mobility restrictions (i.e. a ratio below 2). They are: Denmark, Finland and Sweden in the European group; South Korea, Mongolia, Papua New Guinea and Afghanistan in the Asian group; Benin, Botswana, Burkina Faso, Togo and Yemen in the African group; and Uruguay in the Americas.
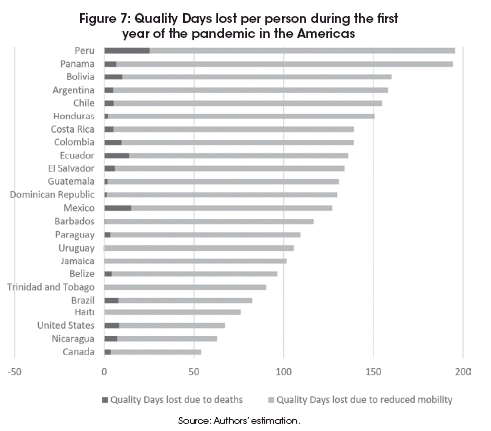
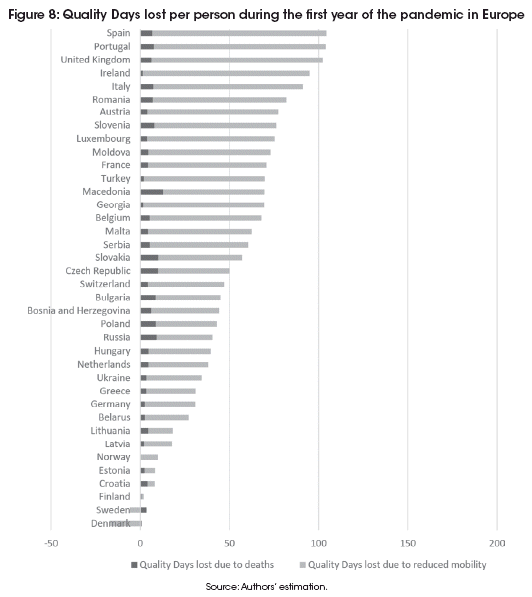
In Figures 7 to 10 we have plotted the average loss of Quality Days per person during the first year of the pandemic for each country on each continent, distinguishing between Quality Days lost to COVID-19 related deaths and Quality Days lost to reduced mobility.
To facilitate comparison across continents, the scales are identical on each graph, ranging from -50 QD to 200 QD lost per person during the first year of the pandemic. Within every regional group we see a very wide variety of outcomes. Almost everywhere, most of the Quality Days lost are due to restrictions in mobility, and these restrictions are not always by force, but frequently by choice, as can be seen from the outcome in countries with few legally imposed restrictions.
On every continent, there is at least one country whose central government decided that there was no need to make too much of a fuss about this pandemic, and thus let people do as they please.
In the Americas, this was the case in Brazil, which has suffered the second highest number ofCOVID-19 deaths in the world, and a significant voluntary reduction in mobility (20% on average over the first year of the pandemic). It was also to a large extent the case in the United States, where restrictions varied by state, and were not enforced, and resulted in an average reduction in mobility of only 16% over the first year of the pandemic, and also the largest number of COVID-19 related deaths. Still, these two countries lost fewer Quality Days per person than most other countries in the region.
Sweden was the famously "rogue" country in the European group. It experienced two big waves of deaths, reaching 960 excess deaths per million by 11 March 2021. Most were among the very aged, however, and in terms of lost Quality Days per person, Sweden is found among the lowest in Europe. Indeed, along with Denmark it had a negative loss of Quality Days per person. Spain, Portugal and the United Kingdom, on the other hand, all lost more than 100 Quality Days per person during the first year of the pandemic.
South Africa is the country in the Africa region that has suffered by far the most deaths, reaching 2,241 excess deaths per million inhabitants by 11 March 2021. This is showed in the dark red part of Figure 9. However, both South Africa, and all other countries on the continent suffered a lot more from reduced mobility. The most famous "rogue" country on the continent is probably Tanzania, whose president did not want to curtail economic activity, and did not even try to secure vaccines, but died in March 2021, with widespread suspicion that the cause was COVID-19. Still, the country lost only 23 Quality Days per person during the first year of the pandemic.
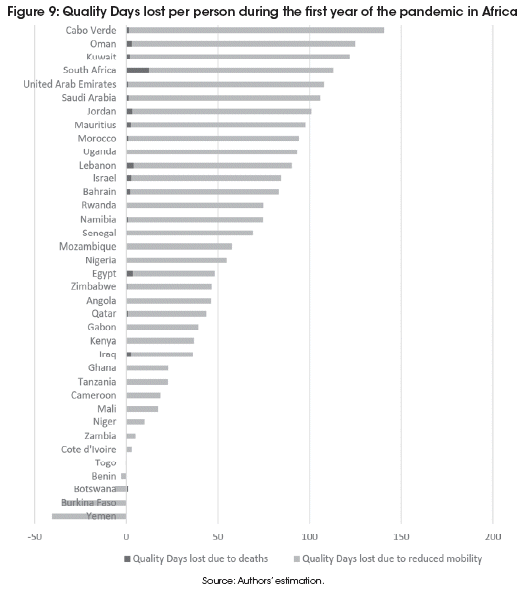
Countries in Asia have generally been doing exceptionally well at avoiding COVID-19 deaths. The worst hit country was Kazakhstan reaching 1,699 excess deaths per million by 11 March 2021. Neighboring Kyrgyzstan and Tajikistan also got hit hard, but other countries in the region have seen few COVID-19 deaths compared to the rest of the world. Still, the Philippines has lost almost 150 Quality Days due to strongly reduced mobility during the first year of the pandemic. India, Malaysia, Myanmar and Sri Lanka also lost more than 100 Quality Days per person, despite very low death rates.
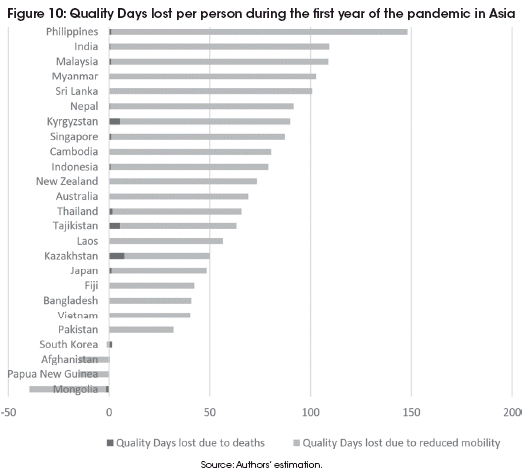
The newly released World Happiness Report 2021 focuses on the effects COVID-19 has had on peoples lives around the world. Based on the surveys carried out worldwide by Gallup every year, it reports changes in life satisfaction between 2017-2019 and 2020 for 95 countries (see Helliwell et al. (2021), Table 2.2). Surprisingly, they do not find a reduction in global happiness during the pandemic. What they do find, however, is a statistically significant increase in life satisfaction in East Asia, South Asia and Sub-Saharan Africa, and a significant decrease in Latin America. In other regions changes were insignificant. The Philippines, however, saw the biggest drop in life satisfaction of any country in the World, which is consistent with our finding that it is among the countries with the biggest welfare losses during the first year of the pandemic (Panama and Peru were not surveyed in 2020).
It is also important to remember that while men lost about 45% more life years than women due to COVID-19 in 2020 (Pifarré-i-Arolas etal., 2021), the mobility of women and young people were reduced more than it was for men and older people (Caselli et al. (2021). Thus, if the loss of wellbeing from reduced mobility is at least an order of magnitude larger than the loss ofwellbeing from COVID-19 deaths, then we would expect women and young people to have suffered bigger reductions in welfare than men and older people, which is consistent with the findings in Helliwell et al. (2021).
5. Putting COVID-19 into perspective
In this section, we will put the effects of the COVID-19 pandemic further into perspective, both in terms of life years lost and setbacks in the quality of life.
As shown in the previous section, just 30 countries accounted for about 87% of all life years lost due to COVID-19 during the first year of the pandemic, and no country lost more than 0.2% of their remaining life years. This means that the vast majority of countries have seen a limited loss of life so far. The global loss of life years during the first year of the pandemic amounted to approximately 48 million life years, which is a relatively small number. Every year, at least twice as many life years are lost due to children dying of diarrhea14, although typically not in the same countries as people are dying of COVID-19. During the first year of the pandemic, COVID-19 related excess deaths accounted for 3-4% of all lost life years15.
Another way of putting COVID-19 deaths into perspective is to compare the 48 million life years lost to COVID-19 to the number of life years added simply through babies being born. During 2020, about 140 million children were born across the world, with an average life expectancy of about 72.6 years16, meaning that about 10 billion life years were added to the global stock. Thus, for every life year lost to COVID-19, we gained about 208 life years from babies being born. On an average day, we gain about 28 million life years just by babies being born. This means that the 48 million life years lost to COVID-19 during the first year of the pandemic have set us back less than 2 days.
It is more difficult to put the DLife dimension of the pandemic into perspective, as we have not experienced anything even remotely similar during our lifetimes. The costs of the lockdowns have been astronomical and multidimensional, with simultaneous shocks on both the supply side and the demand side of the world economy. ILO (2020) calculated that the equivalent of 400 million full-time jobs were lost worldwide during the second quarter of 2020, compared to the same quarter the year before. Few governments have been able to compensate workers and business owners for their lost income during the pandemic, so hundreds of millions of families have seen incomes drop dramatically. Lakner et al. (2020) estimate that the COVID-19 pandemic is likely to have pushed between 88 and 115 million people into extreme poverty in 2020. Decerfet al. (2020) estimate that 235 million additional poverty years have been generated by our responses to the pandemic, thus reversing decades of steady progress in poverty reduction. The World Bank (2020b) estimates that the ongoing crisis will erase almost all the progress made during the last five years in terms of poverty reduction.
The OECD forecasts that global GDP will fall by 4.5% in 2020, compared to 2019. In Italy, India, Mexico, UK, and France the contraction is forecast to be more than double that (Armstrong, 2020). Since global GDP normally increases by a bit more than 2% per year, this means a three-year setback in global GDP due to our reactions to the pandemic.
According to the United Nations, "the COVID-19 pandemic has created the largest disruption of education systems in history, affecting nearly 1.6 billion learners in more than 190 countries and all continents". They argue that "the crisis is exacerbating pre-existing education disparities by reducing the opportunities for many of the most vulnerable children, youth, and adults", and that "closures of educational institutions hamper the provision of essential services to children and communities, including access to nutritious food, affect the ability of many parents to work, and increase risks of violence against women and girls" (United Nations, 2020).
While children can potentially catch up on missed learning in the future, the gaps that are opening up between privileged and disadvantaged students will be very difficult to close. Privileged students with good Internet access, private teachers, appropriate spaces to study, and strong self-motivation will likely continue to do fine despite closed schools and quarantine. However, disadvantaged children without Internet, without food, and without personal space, will find it almost impossible to advance with their study program. In any future admissions tests, interviews or competitions, the latter will have little chance of competing with the former, so the disadvantaged children (the majority) will suffer permanent setbacks from these school closures. Hopefully, the pandemic will at least provide a natural experiment that will allow future researchers to test the impact of public education systems on inequality, both in poor countries and richer countries.
There have also been huge setbacks in terms of public health, as regular public health interventions have been interrupted. The World Health Organization highlights that "preliminary data for the first four months of 2020 points to a substantial drop in the number of children completing three doses of the vaccine against diphtheria, tetanus and pertussis (DTP3). This is the first time in 28 years that the world could see a reduction in DTP3 coverage -the marker for immunization coverage within and across countries". They warn that "the avoidable suffering and death caused by children missing out on routine immunizations could be far greater than COVID-19 itself" (World Health Organization, 2020b).
Mental health is a critical part of overall health and well-being, and, according to a recent global survey by the WHO, mental health services have suffered major disruptions at a time when they are much needed (World Health Organization, 2020c). Isolation, separation from loved-ones, bereavement, loss of income, uncertainty, and fear can all trigger or exacerbate adverse mental health conditions. This can lead to increased levels of alcohol and drug use, insomnia, anxiety, or even suicide. The Economist recently carried out a survey of early signs of increases in suicide due to COVID-19 and found the signs to be ominous. For example, a CDC survey carried out last summer showed that one in four young adults had considered taking their own life. Some suicide hotlines in the US have seen an eightfold-increase in calls. Japan and Nepal have already reported increases in suicides of 15% and 20%, respectively, while Thailand fears an increase of more than 30% this year. Since it takes time for lives to unravel completely, suicide experts expect the tolls to be much worse in 2021 (The Economist, 2020b).
Even the countries that have managed the pandemic relatively well, with few deaths and minimal lockdowns, are suffering the economic consequences of the pandemic in other parts of the world. Japan, for example, has seen extremely low COVID-19 mortality, despite early seeding of the virus, despite relatively modest constraints on human interaction, and despite having the worlds oldest population and the worlds most populous city. But, since Japan is the worlds third biggest exporter, the recession in the rest of the World has had a dramatic effect on exports, and Japan is currently suffering the biggest slump on record (BBC News, 2020a). New Zealand briefly managed to eliminate the virus, but at a huge cost, as they have had to seal off the island country (BBC News, 2020b). They are now battling the deepest recession since at least 1987, when the current system of measurement began (BBC News, 2020c) and borders are still closed to all but the most critical travel.
Probably the worst hit sector of all is the global tourism sector. The United Nations World Tourism Organization recently released a report (UNWTO, 2020) on the devastating impacts the pandemic has had on the sector:
100-120 million jobs at risk
Loss of around USD 1 billion in exports from tourism
International tourism set back about 20 years
Devastating impacts on small island developing states highly dependent on tourism.
6. Conclusions and recommendations
This paper has reviewed the impacts ofCOVID-19, and our response, for 124 countries in the world in terms of both excess deaths and changes in the quality of life during the first year of the COVID-19 pandemic (until 11 March 2021). Given that the SARS-CoV-2 virus spread quickly to every corner of the world (it even got to Antarctica)17, the diversity of experiences is astounding, and worth learning from.
Our main conclusion is that there is no trade-off between life and death, economy and health, or livelihoods and lives, because the countries that did worst in one dimension also did worst in the other dimension. Peru was the hardest hit country in the world during the first year of the pandemic, with 4,442 excess deaths per million people by 11 March 2021 while also suffering an average reduction in daily mobility of 47% over the whole year, which is the second highest in the world. In total Peru lost 196 Quality Days of life per person during the first year of the pandemic, 170 of which were due to mobility restrictions and 26 of which were due to COVID-19 related deaths. At the other end of the spectrum we find Denmark, Norway, Finland, South Korea and Mongolia with no significant excess deaths nor mobility reductions during the first year of the pandemic. Even Sweden, which avoided lockdowns altogether, did not implement any serious system of testing and contact tracing, and did not even recommend mask wearing in public, has done quite well in the cross country comparison.
Across the world, we calculate that about 48 million life years were lost during the first year of the pandemic, corresponding to 0.018% of all expected life years. For comparison, at least double the amount of life years are lost every year due to children dying of diarrhea. About 28 million life years are created every day from babies being born, so the first year of the pandemic set us back less than two days in terms of quantity of life. The setbacks in terms of quality of life are several orders of magnitude larger. Some countries have suffered close to a 50% reduction in mobility sustained over 12 months, with devastating effects on many aspects of quality of life. We estimate that 1.2 billion quality life years were lost due to mobility reductions, which is 25 times as many as life years lost due to COVID-19 related deaths during the first year of the pandemic.
The sharp contrast between the relatively modest losses of quantity of life and the huge losses in quality of life suggests that our reactions to the pandemic have been disproportionate, with the cure causing significantly more harm than the disease at the global level.
6.1. What we should have done: Prevention
Prevention is always the first choice in disaster risk management. Approximately 60% of all human infectious diseases are zoonoses, meaning diseases that originate in animals (Fathke, 2013). We could have significantly reduced the risk of a lethal zoonotic virus appearing by not killing and eating billions of wild or domesticated animals every single day (Zampa, 2018).
Short of the whole world going vegan, we should at the very least be carefully monitoring emerging zoonotic viruses, and pay attention to these warnings. For example, Menachery et al. (2015) warned in the title of their 2015 paper that "A SARS-like cluster of circulating bat coronaviruses shows potential for human emergence". Global monitoring networks exist, and with new digital technologies they can be made vastly more efficient (Milinovich et al., 2014). These global structures have been quite successful at managing many recent threats, such as the original MERS-CoVof 200318, the 2009 H1N1 flu pandemic19, the 2012 MERS-CoV20, and the 2014-2016Ebola outbreak21.
The countries that reacted immediately to the early warnings coming out of China about a novel Coronavirus, and quickly ramped up testing capacity in order to facilitate widespread early screening, isolation and contact tracing, were able to detect and contain outbreaks without the need for lockdowns, school closures or other major interruptions of everyday life while at the same time preventing excess deaths. South Korea, Taiwan, Vietnam, Singapore, Hong Kong, and Iceland are examples of countries that successfully applied this ideal strategy.
The world would have avoided millions of deaths and there would be at least a hundred million fewer people living in poverty by the end of this year, if all countries had reacted like them.
Countries that did not react quickly, but only started worrying when the WHO belatedly declared COVID-19 a pandemic on 11 March 2020, completely missed the opportunity to apply this ideal strategy of handling the virus. Once the virus was spreading widely in communities across the world, mostly by asymptomatic individuals, the optimal strategy of screening, contact tracing, isolation and eradication became infeasible.
6.2. What we need to do now: total harm reduction
At this point in time, with about half a million new COVID-19 cases being officially recorded every day, and many millions of undetected cases undoubtedly occurring as well, we have to switch to a new strategy of total harm reduction. However difficult it is, we have to acknowledge that we failed at containing and suppressing the SARS-CoV-2 virus, and that trying to do so at this point in time will probably cause more harm than the virus itself would cause. Lets be thankful that this time the infection fatality rate turned out to be much lower than initially feared (Ioannidis, 2020), and lets pledge to do much better next time.
Total harm reduction requires a holistic, global approach to dealing with the pandemic, as all our decisions have far reaching effects on every aspect of life across the world. Epidemiologists are extremely important for doing what we should have done (as outlined in section 6.1 above), but their field of expertise is too narrow for dealing with what now needs to be done. For that purpose, public health experts are much better positioned, as they are trained to take into account the multiple dimensions of a health crisis, including psychological effects, long term developmental impacts on children, and effective methods of communication and community engagement. For an even broader view of the diverse indirect effects and tradeoffs across sectors and across borders, economics training is needed. We should definitely listen to the scientists and the experts, but to get the full perspective and move towards total harm reduction, we have to make sure to include a broad range of experts, from many different disciplines and parts of the world.
Our recommendations, after reviewing the evidence presented in this paper and after having lived through one of the strictest lockdowns in the world, with one of the highest per capita fatality rates, are the following:
First, lets immediately work to optimize the immune system of every single person, so that it can fight the virus as effectively as possible, and in this way avoid the need for hospitalization, and prevent death. In the short run, this means providing key nutritional supplements, especially vitamins A, C, D, E, B2, B6, B1 2, folic acid, iron, selenium, and zinc. In the medium term it means promoting access to healthy and nutritious diets, as well as active lifestyles with plenty of access to nature (Macciochi, 2020). We should all look to Japan for inspiration, as they have the longest life-expectancy in the world, and their COVID-19 infection fatality rate is close to 0 despite widespread COVID-19 infection. Boosting the immune system also means reducing extreme stress (McLeod, 2010). Asking rich people to work from their comfortable homes with gardens and Internet and not go to the theater for some months is relatively harmless, but locking up self-employed people or daily workers in poor countries, preventing them from earning money for food and shelter, is just cruel. Suicides due to economic despair are expected to increase dramatically around the world during 2021 (The Economist, 2020b).
Second, we should absolutely prioritize getting all children back in school. Quality public education is our most important strategy for reducing inequality of opportunity and promoting long-run sustainable development across the world. Even mediocre public education can be a life-line for disadvantaged children, providing much needed meals and protection from domestic violence. Children are at extremely low risk of a bad COVID-19 outcome, and scattered evidence suggests that schools are not important drivers of infection and death (Couzin-Frankel, Vogel and Weiland, 2020). Sweden and Bolivia both have close to 11 million inhabitants, but have implemented diametrically opposite school strategies during the pandemic, with very different outcomes. Sweden didn't close schools, nor made children wear masks or socially distance, whereas in Bolivia the whole school year was cancelled22 and there have been no in-person classes at all since mid-March 2020. Despite this, just in La Paz, one of the nine states in Bolivia, at least 80 teachers died from COVID-19 during the first wave with the strictest lockdown23. In contrast, Vogel (2020) identified only a handful of cases of Swedish teachers or school staff having died from COVID-19. Keeping teachers out of schools and away from students is clearly not enough to keep them safe from COVID.
Third, we have to insist on the importance of physical distancing, hand hygiene, masks, ventilation and other simple, cheap and sustainable measures of reducing the spread of the virus and reducing the viral load received by those infected. For the foreseeable future, we have to curb our natural reflexes to shake hands, hug, or kiss cheeks, and instead bow or bump elbows. We have to clean our hands before and after touching a potentially infected surface, such as a supermarket cart, a cash machine, or a door handle. We have to wear masks in public transportation, supermarkets, banks, and other places where a lot of strangers gather and cannot maintain physical distance. Big, indoor crowds should be prohibited in order to avoid potential super-spreader events.
It is important that all these measures are tolerable over quite a long time. If we put too many restrictions on people, their social activities will be driven underground, with potentially adverse effects. For example, a 9 pm curfew may easily backfire, as young people, who perceive almost no risk from COVID-19, might organize sleep-over house parties from 9 pm to 9 am behind closed doors and windows, instead of going out for a few hours with a few friends to a well-ventilated restaurant or bar with good hygiene and physical distancing. As much social interaction and physical activity as possible should be done outdoors, so prohibiting people from jogging in parks, taking their toddlers to playgrounds, hiking in nature, or playing tennis, is clearly counter-productive. All of this was prohibited in Bolivia during the first six months of the pandemic.
Fourth, we need to promote more balanced communication about this pandemic. Peter Drucker once said "You can't manage what you don't measure", and that is very true. But if one issue gets measured and reported in excruciating detail every hour of every day while other equally important issues get measured annually with several years of delay, that will inevitably distort priorities. When Lauren Gardner, associate professor at the Department of Civil and Systems Engineering at Johns Hopkins Whiting School of Engineering, created the absolutely brilliant interactive web-based COVID-19 dashboard to track the coronavirus outbreak across the world in real time24, there is no way she could have foreseen the catastrophic unintended side-effects it would have. Having access to enormous amounts of data in such a user-friendly and visually attractive format, but without context and perspective, caused news media, governments, and the public in general to panic and react disproportionately, depriving billions of children of education and interaction with their friends, causing hundreds of millions of people to lose their jobs or their small businesses, and causing hundreds of millions of people to be plunged into poverty.
Extreme precautions were indeed warranted at the beginning of the pandemic when case fatality rates appeared very high. But by now it is abundantly clear that the vast majority of infections are asymptomatic, that lockdowns are either ineffective or outright counterproductive, and that we urgently need a more holistic perspective that takes into account all aspects of peoples lives, so that we can implement policies that minimize total harm and not just COVID-19 cases.
The change of direction necessary is an extremely bitter pill to swallow for many people, because it means that we have to admit that our obsession with controlling the spread of the virus has done much more harm than the virus itself will ever do. But we really have to swallow this unpleasant pill in order to save the world and get back on track to advance our goals of eliminating poverty and hunger, providing quality education for all, reducing inequality, solving the problem of climate change, etc.
Notes
* Executive Director, Sustainable Development Solutions Network Bolivia
Contact: lykke.e.andersen@sdsnbolivia.org
** Assistant Director, Sustainable Development Solutions Network Bolivia
Contact: alejandra.gonzales@sdsnbolivia.org
*** An earlier version of this paper was prepared for the 57th Annual Conference of the Japan Society for Social Science on Latin America, 14-15, November 2020. The authors are extremely grateful to Fundación Solydes for supporting our work at SDSN Bolivia throughout this pandemic. We also thank Benoît Decerf, Francisco H. G. Ferreira, Daniel G. Mahler and Olivier Sterck for kindly sharing their calculations on average life years lost per COVID-19 death for 150 different countries in the World. We highly appreciate the comments and suggestions received from Stefano Canelas, Jesper Lindholt, Daniel G. Mahler and an anonymous referee on earlier drafts of the paper.
1 See Microbiology by numbers (2011).
2 Fora general overview of the immune system, see for example Maggini, Pierre and Calder (2018).
3 See https://www.euromomo.eu/.
4 SeeWu, McCann, Katz, Peltier and Deep Singh (2020).
5 See The Economist (2020a).
6 FT Visual & Data Journalism Team (2020).
7 The authors use the World Bank's income class poverty thresholds, as derived by Jolliffe and Prydz (2016), namely $1.90 per person per day in low-income countries (LICs); $3.20 a day in lower-middle-income countries (LMICs); $5.50 a day in upper-middle-income countries (UMICs); and $21.70 a day in high-income countries (HICs).
8 See the World Bank's World Development Indicator on Mobile Cellular Subscriptions (per 100 people): https://data.worldbank.org/indicator/IT.CEL.SETS.P2
9 They use the daily values calculated by Arroyo Marioli et al. (2020), updated daily here: http://trackingr-env.eba-9muars8y.us-east-2.elasticbeanstalk.com/.
10 Calculated as the average daily reduction in visits to retail outlets and recreation, visits to grocery stores and pharmacies, visits to transit stations, and visits to workplaces from March 4 to May 1 2, 2020, according to the Google (2020) Community Mobility Reports (https://www.google.com/covid19/mobility/).
11 See https://www.worldometers.info/coronavirus/.
12 See https://ourworldindata.org/coronavirus.
13 Official COVID-1 9 deaths outside the 1 24 countries included in our analysis account for less than 5% of the total confirmed global COVID-1 9 deaths during the first year of the pandemic, but we have added 4.1% to reach the global total of 48 million lost life years due to COVID-19 during the first year of the pandemic.
14 According to Our World in Data, 1.57 million people (mostly young children) died of diarrheal diseases in 2017 (https://ourworldindata.org/causes-of-death). Conservatively assuming that each of these deaths implies on average 64 life years lost, this sums to about 100 million life years lost to diarrhea every year.
15 Assigning conservative estimates of lost life years to each cause of the approximately 54 million deaths that take place every year (e.g. 40 years lost for each traffic fatality, 15 years lost for a death due to cancer, liver disease, or diabetes, 10 years for dementia, etc.), we calculated a total loss of life years of at least 1400 million life years during a normal year.
16 According to the World Bank's World Development Indicators for 2018 (https://data.worldbank.org/indicator/SP.DYN.LE00.IN).
17 https://www.webmd.com/lung/news/20201224/antarctica-reports-first-covid-19-outbreak
18 SARS-CoV was first detected in Asia in February of 2003. It spread to more than two dozen countries, infected 8,098 persons, of which 9.6% died, before it was successfully contained and eradicated (https://www.cdc.gov/sars/about/fs-sars.html).
19 H1 N1 pdm09 was first reported in California in April of 2009. It had spread to more than 70 countries by June 11, when it was declared a pandemic. About half a million people worldwide died from H1 N1 pdm09 virus infection during the first year, of whom 80% were younger than 65. Vaccines were developed and widely deployed in January of 2010, months after the second wave had come and gone. The H1 N1 pdm09 virus continues to circulate as a seasonal flu virus, killing people every year (https://www.cdc.gov/flu/pandemic-resources/2009-h1n1-pandemic.html, https://www.cdc.gov/h1n1flu/cdcresponse.htm).
20 The first known case of MERS-CoV occurred in Jordan in April of 201 2, likely jumping from camels to humans. With a case fatality rate above 30% it is highly lethal, and has fortunately not managed to spread widely. It has not yet been eradicated, nor is there a treatment or a vaccine available. The biggest outbreak outside the Middle East was in South Korea (https://www.cdc.gov/coronavirus/mers/about/index.html).
21 The Ebola virus was first described in 1976 in what is now the Democratic Republic of Congo, but the biggest Ebola virus outbreak ever experienced started in Guinea in 2014 and spread to other countries in West Africa, infecting around 26 thousand persons and killing 11,325 of them. It still exists in DRC to this date. With an average case fatality rate of close to 50%, the virus is highly lethal, and only spreads through the bodily fluids of an infected person, which means that outbreaks can be controlled with solid public health measures (https://www.cdc.gov/vhf/ebola/index.html).
24 See https://coronavirus.jhu.edu/map.html.
Fecha de recepción: 25 de enero de 2021
Fecha de aceptación: 5 de abril de 2021
Manejado por ABCE/SEBOL/IISEC
References
1. Abu Raddad, L. J., Chemaitelly, H., Ayoub, H. H., Al Kanaani, Z., Al Khal, A., Al Kuwari, E., … and Bertollini, R. (2020). Characterizing the Qatar advanced-phase SARS-CoV-2 epidemic. Cold Spring Harbor: medRxiv. Preprint. https://doi.org/10.1101/2020.07.16.20155317
2. Amorim Filho, L., Szwarcwald, C. L., Mateos, S. D. O. G., De Leon, A. C. M. P., De Andrade Medronho, R., Veloso, V. G., ... and Werneck, G. L. (2020). Seroprevalence of IgG and IgM anti-SARS-CoV-2 among voluntary blood donors in Rio de Janeiro, Brazil. Revista de Saúde Pública; 54(69). Retrieved: https://www.researchgate.net/publication/342816781_Seroprevalence_of_anti-SARS-CoV-2_among_blood_donors_in_Rio_de_Janeiro_Brazil
3. Armstrong, M. (2020). How Hard Will GDP Be Hit in 2020? Statista, Economy (Published 16 September 2020). https://www.statista.com/chart/21961/oecd-gdp-growthprojections-2020-on-2019/ [ Links ]
4. Arroyo Marioli, F., Bullano, F., Kučinskas, S. and Rondón-Moreno, C. (2020). Tracking R of COVID-19: A New Real-Time Estimation Using the Kalman Filter (SSRN Scholarly Paper Nº ID 3581633). Social Science Research Network, Rochester, NY. https://papers.ssrn.com/sol3/papers.cfm?abstract_id=3581633. [ Links ]
5. Bargain, O., and Ulugbek, A. (2020). Poverty and COVID-19 in Developing Countries (Bordeaux University, Economics Working Papers 2020-08). Groupe de Recherche en Economie Theorique et Appliquee (GREThA). https://ideas.repec.org/p/grt/bdxewp/2020-08.html
6. Basu, A. M., Basu, K. and Tapia, J. M. U. (2020). The complexity of managing COVID-19: How important is good governance? Brookings Report. https://www.brookings.edu/research/the-complexity-of-managing-covid-19-how-important-is-good-governance/ [ Links ]
7. BBC News (2020a). Coronavirus: Japan suffers its biggest economic slump on record. Published 17 August 2020. https://www.bbc.com/news/business-53802967.
8. ---------- (2020b). New Zealand lifts all COVID restrictions, declaring the nation virusfree. Published 8 June 2020. https://www.bbc.com/news/world-asia-52961539.
9. ---------- (2020c). COVID pushes New Zealand into worst recession in years. Published 17 September 2020. https://www.bbc.com/news/business-54186359.
10. Beach, B., Clay, K. and Saavedra, M. H. (2020). The 1918 influenza pandemic and its lessons for COVID-19 (NBER Working Paper Series, Nº 27673). National Bureau of Economic Research. https://www.nber.org/system/files/working_papers/w27673/w27673.pdf
11. Buss, L. F., Prete Jr., C. A., Abrahim, C. M. M., Mendrone Jr. A., Salomon, T., De Almeida-Neto, C., ... and Sabino, E. C. (2020). COVID-19 herd immunity in the Brazilian Amazon. Cold Spring Harbor: medRxiv. Preprint. https://doi.org/10.1101/2020.09.16.20194787
12. Caselli, F., Grigoli, F., Sandri, D. and Spilimbergo, A. (2021). Mobility under the COVID-19 Pandemic: Asymmetric Effects across Gender and Age. Covid Economics, 64, 135-164. https://cepr.org/file/10211/download?token=ZZzuKAeJ [ Links ]
13. Couzin-Frankel, J., Vogel, G. and Weiland, M. (2020). School openings across globe suggest ways to keep coronavirus at bay, despite outbreaks. Science, 7 July. https://www.sciencemag.org/news/2020/07/school-openings-across-globe-suggest-ways-keepcoronavirus-bay-despite-outbreaks [ Links ]
14. Decerf, B., Ferreira, F. H., Mahler, D. G. and Sterck, O. (2020). Lives and Livelihoods: Estimates of the Global Mortality and Poverty Effects of the COVID-19 Pandemic (Policy Research Working Paper Nº 9277). World Bank Group, Development Research Group. http://documents1.worldbank.org/curated/en/655511592232527722/pdf/Lives-and-Livelihoods-Estimates-of-the-Global-Mortality-and-Poverty-Effects-of-the-COVID-19-Pandemic.pdf
15. Dicker, D., Nguyen, G., Abate, D., Abate, K. H., Abay, S. M., Abbafati, C., … and Abdelalim, A. (2018). Global, regional, and national age-sex-specific mortality and life expectancy, 1950-2017: a systematic analysis for the Global Burden of Disease Study 2017. The Lancet, 392 (10159), 1684-1735.
16. Dong, E., Du, H. and Gardner, L. (2020). An interactive web-based dashboard to track COVID-19 in real time. The Lancet, Infectious Diseases, 20(5), 533-534. https://www.thelancet.com/journals/laninf/article/PIIS1473-3099(20)30120-1/fulltext [ Links ]
17. ECDC (2020). Timeline of ECDC’s response to COVID-19. European Centre for Disease Prevention and Control. https://www.ecdc.europa.eu/en/COVID-19/timeline-ecdcresponse
18. Fathke, R. (2013). Food Animal Production, Zoonotic Disease, and Global Security. The Stimson Center, Commentary, 11 June. https://www.stimson.org/2013/food-animalproduction-zoonotic-disease-and-global-security/ [ Links ]
19. Fontanet, A., Tondeur, L., Madec, Y., Grant, R., Besombes, C., Jolly, N., ... and Hoen, B. (2020). Cluster of COVID-19 in northern France: a retrospective closed cohort study. Cold Spring Harbor: medRxiv. Preprint. https://doi.org/10.1101/2020.04.18.20071134 [ Links ]
20. FT Visual & Data Journalism Team (2020). Coronavirus tracked: the latest figures as countries fight COVID-19 resurgence. Financial Times. https://www.ft.com/content/a2901ce8-5eb7-4633-b89c-cbdf5b386938. [ Links ]
21. Gavi (2020). The COVID-19 vaccine race. The Vaccine Alliance. Updated 15 December 2020. https://www.gavi.org/vaccineswork/covid-19-vaccine-race [ Links ]
22. Google (2020). Community Mobility Reports. Google. www.google.com/COVID19/mobility/ [ Links ]
23. Helliwell, J. F., Layard, R., Sachs, J. D., De Neve, J.-E., Aknin, L. B. and Wang, S. (2021). World Happiness Report 2021. https://worldhappiness.report/ [ Links ]
24. Hibino, S., Hayashida, K., Ahn, A. C. and Hayashida, Y. (2020). Dynamic Change of COVID-19 Seroprevalence among Asymptomatic Population in Tokyo during the Second Wave. Cold Spring Harbor: medRxiv. Preprint. https://doi.org/10.1101/2020.09.21.20198796. [ Links ]
25. ILO (2020). ILO Monitor: COVID-19 and the world of work. Fifth edition Updated estimates and analysis. International Labour Organization. https://www.ilo.org/w”cmsp5/groups/public/@dgreports/@dcomm/documents/briefingnote/wcms_749399.pdf
26. Ioannidis, J. P. A. (2020). Infection fatality rate of COVID-19 inferred from seroprevalence data. Bulletin of the World Health Organization, Article ID: BLT.20.265892. https://www.who.int/bulletin/online_first/BLT.20.265892.pdf [ Links ]
27. Javed, W., Baqar, J., Abidi, S. H. B. and Farooq, W. (2020). Seroprevalence findings from metropoles in Pakistan: implications for assessing COVID-19 prevalence and casefatality within a dense, urban working population. Cold Spring Harbor: medRxiv. Preprint. https://doi.org/10.1101/2020.08.13.20173914 [ Links ]
28. Jolliffe, D. and Prydz, E. B. (2016). Estimating international poverty lines from comparable national thresholds (Policy Research Working Paper Nº 7606). World Bank. https://openknowledge.worldbank.org/handle/10986/24148
29. Karlinsky, A. and Kobak, D. (2021). The World Mortality Dataset: Tracking excess mortality across countries during the COVID-19 pandemic. Cold Spring Harbor: medRxiv. Preprint. https://www.medrxiv.org/content/10.1101/2021.01.27.21250604v1 [ Links ]
30. Lakner, C., Yonzan, N., Mahler, D. G., Castaneda Aguilar, R. A., Wu, H. and Fleury, M. (2020). Updated estimates of the impact of COVID-19 on global poverty: The effect of new data. The World Bank, Data Blog, 7 October. https://blogs.worldbank.org/opendata/updated-estimates-impact-covid-19-global-poverty-effect-new-data
31. Macciochi, J. (2020). Immunity: The Science of Staying Well. Thorsons. [ Links ]
32. Maggini, S., Pierre, A., and Calder, P. C. (2018). Immune Function and Micronutrient Requirements Change over the Life Course. Nutrients, 10(10), 1531. https://doi.org/10.3390/nu10101531 [ Links ]
33. Malani, A., Shah, D., Kang, G., Lobo, G. N., Shastri, J., Mohanan, M., ... and Kolthur-Seetharam, U. (2020). Seroprevalence of SARS-CoV-2 in slums and non-slums of Mumbai, India, during June 29-July 19, 2020. Cold Spring Harbor: medRxiv. Preprint. https://doi.org/10.1101/2020.08.27.20182741
34. McLeod, S. A. (2010). Stress, illness and the immune system. Simply Psychology. https://www.simplypsychology.org/stress-immune.html [ Links ]
35. Menachery, V. D., Yount, B. L., Jr., Debbink, K., Agnihothram, S., Gralinski, L. E., Plante, J. A., Graham, R. L., Scobey, T., Ge, X. Y., Donaldson, E. F., Randell, S. H., Lanzavecchia, A., Marasco, W. A., Shi, Z. L. and Baric, R. S. (2015). A SARS-like cluster of circulating bat coronaviruses shows potential for human emergence. Nature medicine, 21(12), 1508-1513. https://doi.org/10.1038/nm.3985 [ Links ]
36. Microbiology by numbers (2011). Nature Reviews Microbiology, 9, 628. https://doi.org/10.1038/nrmicro2644
37. Milinovich, G. J., Williams, G. M., Clements, A. C. A. and Hu, W. (2014). Internet-based surveillance systems for monitoring emerging infectious diseases. The Lancet, Infectious Diseases, 14(2), 160-168. https://doi.org/10.1016/S1473-3099(13)70244-5 [ Links ]
38. Murray, C. J. L., López, A. D., Chin, B., Feehan, D. and Hill, K. H. (2006). Estimation of potential global pandemic influenza mortality on the basis of vital registry data from the 1918-20 pandemic: a quantitative analysis. The Lancet, 368(9554), 2211-2218. [ Links ]
39. Pifarré-i-Arolas, H., Acosta, E., López-Casasnovas, G., Lo, A., Nicodemo, C., Riffe, T. and Myrskylä, M. (2021). Years of life lost to COVID-19 in 81 countries. Nature Scientific Reports, 11, 3504. https://www.nature.com/articles/s41598-021-83040-3 [ Links ]
40. Rosenberg, E. S., Tesoriero, J. M., Rosenthal, E. M., Chung, R., Barranco, M. A., Styer, L. M. … and Zucker, H. A. (2020). Cumulative incidence and diagnosis of SARS-CoV-2 infection in New York. Annals of Epidemiology, 48, 23-29.e4. https://doi.org/10.1016/j.annepidem.2020.06.004.(http://www.sciencedirect.com/science/article/pii/S1047279720302015
41. Roser, M., Ritchie, H., Ortiz-Ospina, E. and Hasell, J. (2020). Coronavirus pandemic (COVID-19). Published online at OurWorldInData.org. https://ourworldindata.org/coronavirus [ Links ]
42. Sachs, J., Schmidt-Traub, G., Kroll, C., Lafortune, G., Fuller, G. and Woelm, F. (2020). The Sustainable Development Goals and COVID-19. Sustainable Development Report. Cambridge: Cambridge University Press. https://s3.amazonaws.com/sustainabledevelopment.report/2020/2020_sustainable_development_report.pdf
43. Shakiba, M., Nazari, S. S. H., Mehrabian, F., Rezvani, S. M., Ghasempour, Z. and Heidarzadeh, A. (2020). Seroprevalence of COVID-19 virus infection in Guilan province, Iran. Cold Spring Harbor: medRxiv. Preprint. https://doi.org/10.1101/2020.04.26.20079244.th [ Links ]
44. Taubenberger, J. K. and Morens, D. M. (2006). 1918 Influenza: the Mother of all Pandemics. Emerging Infectious Diseases, 12(1), 15-22. https://wwwnc.cdc.gov/eid/article/12/1/05-0979_article [ Links ]
45. Taubenberger, J. K., Kash, J. C. and Morens, D. M. (2019). The 1918 influenza pandemic: 100 years of questions answered and unanswered. Science Translational Medicine, 11(502): eaau5485. https://stm.sciencemag.org/content/11/502/eaau5485.full [ Links ]
46. The Economist. (2020a). Tracking COVID-19 excess deaths across countries. Published 2 October 2020. https://www.economist.com/graphic-detail/2020/07/15/tracking-COVID-19-excess-deaths-across-countries.
47. ---------- (2020b). Will the economic and psychological costs of COVID-19 increase suicides? Published 5 October 2020. https://www.economist.com/international/2020/10/05/will-the-economic-and-psychological-costs-of-COVID-19-increase-suicides.
48. United Nations (2020). Policy Brief: Education during COVID-19 and beyond. https://www.un.org/development/desa/dspd/wp-content/uploads/sites/22/2020/08/sg_policy_brief_COVID-19_and_education_august_2020.pdf [ Links ]
49. UNWTO (2020). The impact of COVID-19 on tourism. United Nations World Tourism Organization. August. https://webunwto.s3.eu-west-1.amazonaws.com/s3fspublic/2020-08/UN-Tourism-Policy-Brief-Visuals.pdf [ Links ]
50. Uyoga, S., Ifedayo, M. O., Karanja, H. K., Nyagwange, J., Tuju, J., Wanjiku, P., ... and Marimwe, G. M. (2020). SARS-CoV-2 Sero-surveillance of blood donors in Kenya. Cold Spring Harbor: medRxiv. Preprint. doi: https://doi.org/10.1101/2020.07.27.20162693. [ Links ]
51. Vogel, G. (2020). How Sweden wasted a ‘rare opportunity’ to study coronavirus in schools. Science, 22 May. https://www.sciencemag.org/news/2020/05/how-swedenwasted-rare-opportunity-study-coronavirus-schools.
52. World Bank (2020a). Global Economic Prospects. Washington, DC: The World Bank.
53. ---------- (2020b). Poverty. Washington, DC: The World Bank. https://www.worldbank.org/en/topic/poverty/overview#1
54. World Health Organization (2020a). Thailand: How a Strong Health System Fights a Pandemic. COVID-19: WHO’s Action in Countries | September 2020. https://www.who.int/docs/default-source/coronaviruse/country-case-studies/thailand-c19-casestudy-20-september.pdf ?sfvrsn=d5534183_2&download=true
55. ---------- (2020b). WHO and UNICEF warn of a decline in vaccinations during COVID-19. Published 15 July 2020. https://www.who.int/news-room/detail/15-07-2020-who-and-unicef-warn-of-a-decline-in-vaccinations-during-COVID-19.
56. ---------- (2020c). COVID-19 disrupting mental health services in most countries, WHO survey. Published 5 October 2020. https://www.who.int/news-room/detail/05-10-2020-COVID-19-disrupting-mental-health-services-in-most-countries-who-survey
57. Worldometer (2020). COVID-19 Coronavirus Pandemic. https://www.worldometers.info/coronavirus/. [ Links ]
58. Wu, J., McCann, A., Katz, J., Peltier, E. and Deep Singh, K. (2020). 338,000 Missing Deaths: Tracking the True Toll of the Coronavirus Outbreak. New York Times. https://www.nytimes.com/interactive/2020/04/21/world/coronavirus-missing-deaths.html. [ Links ]
59. Zampa, M. (2018). How Many Animals Are Killed for Food Every Day? Sentient Media, 16 September. https://sentientmedia.org/how-many-animals-are-killed-for-food-everyday/ [ Links ]
Key variables for calculating the impacts on life and death during the first year of the pandemic