Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Accesos
Accesos
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Revista Científica Ciencia Médica
versión impresa ISSN 2077-3323
Rev Cient Cienc Méd vol.23 no.1 Cochabamba 2020
ARTÍCULO ORIGINAL
ARE PULSE WAVE VELOCITY AND ARTERIAL STIFFNESS MARKERS FOR EARLY PRE-CLINICAL ATHEROSCLEROSIS DETECTION IN RESISTANT HYPERTENSIVE PATIENTS?
¿SON LA VELOCIDAD DE LA ONDA DEL PULSO Y LOS MARCADORES DE RIGIDEZ ARTERIAL PARA LA DETECCIÓN PRECOZ DE LA ATEROSCLEROSIS PRECLÍNICA EN PACIENTES HIPERTENSOS RESISTENTES?
Varahabhatla Vamsi1, Basavaprabhu Achappa2, Padmanabh Kamath3, Vaman Kulkarni4, Ingrid Prkacin5
1General Medicine speciality, Zaporozhye State Medical University, Ukraine.
2Department of Medicine, Kasturba Medical College, Affiliated to Manipal Academy of higher education, India
3Department of Cardiology, Kasturba Medical College, Affiliated to Manipal Academy of higher education, India
4Department of Community Medicine, Kasturba Medical College, Affiliated to Manipal Academy of higher education, India
5Department of Internal Medicine, School of medicine, University of Zagreb, University Hospital Merkur, Croatia.
Correspondence to: Varahabhatla Vamsi
Mail: vamsivarahabhatla@ gmail.com
Provenance and arbitration: no commissioner, subjected to external arbitration.
Received for publication: March 3, 2019
Accepted for publication: July 13, 2020
Quote as: Varahabhatla Vamsi, Basavaprabhu Achappa, Padmanabh Kamath, Vaman Kulkarni, Ingrid Prkacin. Are pulse wave velocity and arterial stiffness markers for early pre-clinical atherosclerosis detection in resistant hypertensive patients?. Rev Cient Cienc Med 2020;23(1): 27-31
ABSTRACT
Pulse wave velocity and arterial stiffness are considered gold standard for assessing sub clinical target organ damage. Endothelial dysfunction is directly proportional to development of pre-clinical atherosclerosis. These above-mentioned surrogate markers are relatively higher in patients with uncontrolled or resistant hypertension patients. The objective was to assess if arterial stiffness and pulse wave velocity are also surrogate markers for pre-clinical atherosclerosis development in patients with resistant hypertension. A total of 160 patients with resistant hypertension from Croatia and India were included in the study. Their central blood pressure and other clinical values were assessed using non-invasive device. With the results obtained can conclude that arterial stiffness is an independent marker which is directly proportional to endothelial dysfunction and development of pre-clinical atherosclerosis.
Palabras clave: Aterosclerosis; Enfermedad Cardiovascular; Velocidad de la Onda del Pulso; Rigidez vascular; Presión Arterial Alta.
RESUMEN
La velocidad de la onda del pulso y la rigidez arterial se consideran el estándar de oro para evaluar el daño subclínico de órganos diana. La disfunción endotelial es directamente proporcional al desarrollo de la aterosclerosis preclínica. Estos marcadores sustitutos mencionados anteriormente son relativamente más altos en pacientes con hipertensión no controlada o resistente. El objetivo fue evaluar si la rigidez arterial y la velocidad de la onda del pulso también son marcadores sustitutos del desarrollo de la aterosclerosis preclínica en pacientes con hipertensión resistente. Un total de 160 pacientes con hipertensión resistente de Croacia e India fueron incluidos en el estudio. Su presión arterial central y otros valores clínicos se evaluaron utilizando un dispositivo no invasivo. Con los resultados obtenidos se puede concluir que la rigidez arterial es un marcador independiente que es directamente proporcional a la disfunción endotelial y al desarrollo de aterosclerosis preclínica.
Keywords: Atherosclerosis; Cardiovascular Disease; Pulse Wave Velocity; Vascular Stiffness; High Blood Pressure.
INTRODUCTION
Pulse wave velocity is the current gold standard of assessing arterial stiffness and vascular health. With the increasing age, it is well known that the vascular age also rises correspondingly. Normal biological changes within the arterial vessels due to the effects of oxidative stress, free radical particles and endothelial dysfunction. Endothelial dysfunction is the primitive stage for development of any vascular pathology according to Davignon et al.1 The normal endothelium is regulated and controlled by the release of nitric oxide (NO). The NO is totally responsible for the normal vascular tonus maintenance, with the dilation and normalization of the vessel wall.2 The aortal (elastic typeof artery)or central blood pressure is regarded the accurate measurement than the brachial artery (due to its muscular type) sensitive to several factors producing false positive result.3 Arteriosclerosis along with endothelial dysfunction is the most common pathogenic mechanism for the progression of sub clinical atherosclerosis. The loss of distensability in the arteries or the cushioning effect increases the arterial stiffness and further degrades facilitating in the development of the development. Recently, non-invasive central blood pressure measuring cuff devices have been developed for the assessment of arterial stiffness with the parameters like central blood pressure, pulse pressure, mean arterial pressure, augmentation index and pulse wave velocity.4These novel non invasive measurement techniques make it convenient to assess the above parameters and serve as novel vascular markers in determining early sub clinical atherosclerosis detection and further management by clinicians. Pulse pressure is the difference between systolic and diastolic blood pressure. Mean arterial pressure is defined as the average blood pressure in a single cardiac cycle. Pulse wave velocity is a diagnostic test at which the blood pressure pulse propagates through an artery or an arterial system.
The aim of this study is to assess and determine if arterial stiffness and pulse wave velocity are vascular bio-markers for early pre-clinical atherosclerosis detection in resistant hypertension patients from Croatia and India.
METHODS AND MATERIALS
We prospectively measured the blood pressure values at Merkur University Hospital, Zagreb, Croatia in January 2018 and Kasturba Medical college hospital, Mangalore, India in August 2018 was conducted. Our inclusion criteria were 160 patients (80 from each country) with Resistant hypertension (RH) (resistance to 3 or more drugs, one is diuretic) exclusion criteria being absence of chronic kidney disease, were analyzed. The PWV, mean arterial pressure (MAP), pulse pressure (PP), CBP, brachial pressure (BP systolic and diastolic) were evaluated using the non-invasive Agedio B900 device (Germany).
The diagnosis of RH was made on the (basis of the ESH/ESC classification of resistant hypertension) inability to control the arterial pressure even after using three or more drugs. The drug combinations included angiotensin converting enzyme inhibitors (ACEI), angiotensin II receptor blockers (ARB), beta blockers (BB), calcium channel blockers (CCB) and diuretics (D). Combinations like ACEI+CCB+D and potassium sparing diuretic were preferred in 30% of the patients. We avoided an improper blood pressure measurement by using an suitable cuff size and informed the patients to avoid a heavy
meal, exercise, smoking and alcohol and also allowing the patient to relax 5 minutes prior the assessment in our study following the new guidelines issued by the international society of hypertension in June 2020. An informed consent of the patients was obtained before participation. The study was approved by local institutional ethics committee. Statistical data was processed in SPSS software; significant differences were considered at p<0,01.The obtained data was interpreted in descriptive statistics and scattered plots.
RESULTS
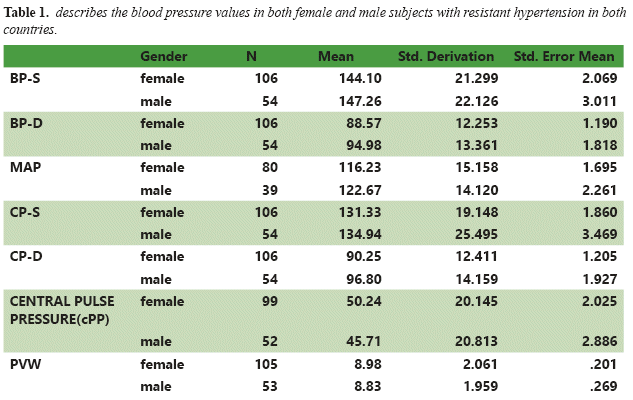
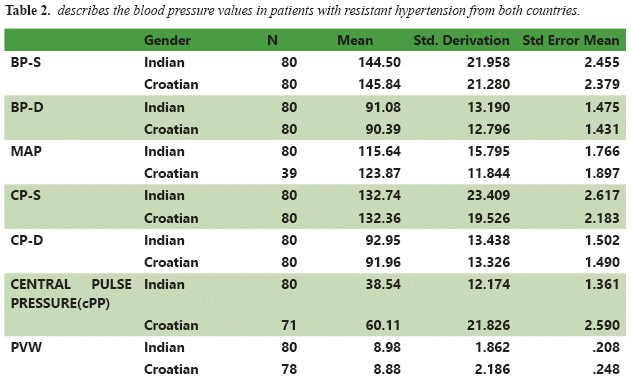
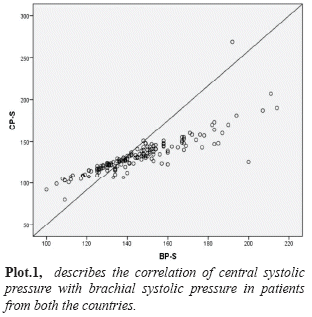
Out of the total 160 patients, 80 (50%) were from India and 80 (50%) from Croatia. The total number of female subjects were 106 (53 were from each country) and males (27 from each country) were 54 respectively. The mean average age was 58.3±13.59; in females (F) 58.83±13.58and 57.58±13.5 in males (M). From the group statistics made gender wise, the values of BP-S, BP-D, MAP, CP-S, CP-D, cPP and PWV have been described in TABLE NO 1. The BP-S values in M/F were 147.26±22.12/144.10±21.29; the BP-D values in M/F were 94.98±13.36/88.57± 12.25 respectively. The MAP values in M/F were122.67±14.12/116.23±15.15 and CP-S values were 134.94±25.49/131.33±19.14 respectively. The CP-D values in M/F were 96.80±14.15/90.25± 12.41 and the cPP was 45.71 ±20.8/50.24±20.14respectively.Thevalues of PWV in M/F were 8.83±1.9/8.98±2.06 m/s. The BP-S values in Indian patients(I)/Croatian patients (C) were144.5±21.9/145.84±21.28; the BP-D values in I/C were 91.08±13.19/90.39±12.7 respectively and have been described in TABLE NO 2. The MAP values in I/C were 115.64±15.7/123.87±11.8 and CP-S values were 132.36±23.4/132.36±19.5 respectively. The CP-D values in I/C were 92.95±13.4/91.96±13.3 and the cPP was 38.5±12.17/60.11 ±21.8 respectively. The values of PWV in I/C were8.98±1.8/8.88±2.1 m/s. The Pearson correlation between CP-S and BP-S was found to be statistically significant p=0.862(see in figure n1). The difference between sexes was statistically significant for PWV (M/F: 8.8/8.9m/s p<0,01).
DISCUSSION
Varahabhatla et al in their prospective study on 80 patients described the effectiveness of PWV and CBP assessment in resistant hypertensive patients and the predictability of hypertension mediated target organ damage.6
Wilkinson et al, described the current possibilities of assessing vasomotor endothelial function. They tested the hypothesis of pulse-wave analysis (PWA) in combination with a provocative pharmacological test might provide an alternative method to assess endothelial dysfunction.7
Lane et al, described the non-invasive tools for establishing pre-clinical atherosclerosis in their review article. Brief data on PWV and pulse wave analysis was evident. Very little is known about the use of PWV in assessing the endothelial dysfunction.8
Sutton et al, in their study on 2488 participants reported that increased aortic pulse wave velocity and arterial stiffness were markers of cardiovascular events in well-functioning older population. Higher levels of arterial stiffness were associated with higher cardiovascular mortality rate and ischemic heart disease.9
Nichols in his review on clinical arterial stiffness assessment using non-invasive waveforms. Higher values of both systolic and pulse pressures resulting in elderly patients or hypertensive patients an increase in circumferential arterial wall stress is evident, which likely causes the breakdown of medial elastin, increasing the possibility of local vascular fatigue, endothelial dysfunction and development of atherosclerosis.10
Mori et al, in their cross-sectional study on 177 Latino and white hypertension population, reported that PWV was associated strongly with carotid intima thickness, proving that PWV assessment in hypertensive population irrespective of ethnicity is an adjunct and independent atherosclerotic marker.11
Terai et al in their longitudinal study on 813 patients described that increase in levels of arterial stiffness as assessed by PWV contributed to an increased incidence of stroke and heart disease, whereas higher reactive hyperaemia evaluation using strain gauge plethysmograph causes a reduced incidence of cardiovascular and cerebrovascular events. PWV is an independent predictor than strain gauge plethysmograph, which showed weak correlation and better outcome.12
Jadhav et al, in their study stated that pulse wave velocity along with flow mediated dilation were the best prediction markers for assessing pre-clinical atherosclerosis and endothelial dysfunction non-invasively. Their study included 102 patients with arterial hypertension and concomitant diabetes who were at high risk for atherosclerosis. High values of arterial stiffness and PWV followed by decreased flow mediated dilation of brachial artery were indicative of non-invasive PWV as a gold standard.13
Kim et al mentioned about the importance of pulse wave velocity and atherosclerosis in his review article. He discussed about the positives of pulse wave velocity inscreening pre-clinical atherosclerosis and cardiac disease prevention on a mass basis. Intensive lifestyle changes, optical risk stratification and therapeutic modulations are necessary for preventing preclinical atherosclerosis and cardiovascular event.14
McEniery et al, in their prospective study on 309 patients described the functioning of endothelium and large artery stiffness development. The results of their study described that even in healthy subjects, reduced endothelial function is strongly associated with not only higher PWV levels, but also pulse pressure and central blood pressure. The results obtained confirm the importance of endothelium dependant nitric oxide and its reduction strongly supporting development of pre-clinical atherosclerosis and increased vascular stiffness.15
CONCLUSIONS
Patients from both the countries did not show any statistical difference in the estimated values. With the non-invasive assessment of PWV and CBP, we can conclude that arterial stiffness is an independent marker which is directly proportional to endothelial dysfunction and development of pre-clinical atherosclerosis. The mechanism of this process is increased PWV and CBP and their contribution in elevating the risk for atherosclerosis development. The vascular age determined by PWV is of utmost importance in assessing the normal endothelial function. We can hypothesise that endothelial dysfunction can be predicted non-invasively with the markers like CBP and PWV, despite of very less evidence. There is a high necessity for future longitudinal and higher population studies to describe the urgency of diagnosing pre-clinical atherosclerosis and validating the non-invasive devices for their regular use in the clinician's office.
REFERENCIAS
1. Davignon J, Ganz P. Role of endothelial dysfunction in atherosclerosis. Circulation. 2004;109:III-27–III-32. Available in: https://doi.org/10.1161/01.CIR.0000131515.03336.f8
2. Anderson TJ, Gerhard MD, Meredith IT, et al. Systemic nature of endothelial dysfunction in atherosclerosis. Am J Cardiol. 1995; 75: 71B–74B. Available in: https://doi.org/10.1016/0002-9149(95)80017-m
3. Shadwick RE. Mechanical design in arteries. J Exp Biol. 1999;202:3305–3313. Available in: https://jeb.biologists.org/content/jexbio/202/23/3305.full.pdf
4. Sueta D, Yamamoto E, Tanaka T, et al. Association of estimated central blood pressure measured non-invasively with pulse wave velocity in patients with coronary artery disease.Int J Cardiol Heart Vasc. 2015;8:52–54. Available in: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5497261/
5. Mancia G, Fargard R, Narkiewicz K, et al.2013 ESH/ESC Guidelines for the management of arterial hypertension: The Task Force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). European Heart Journal, Volume 34, Issue 28, 21 July 2013, Pages 2159–2219. Available in: https://doi.org/10.1093/eurheartj/eht151
6. Vamsi V, Golub A, Pezić M, Fekete P, Findri P, Prkačin I. Central blood pressure and pulse wave velocity in patients with resistant hypertension.Signa Vitae. 2018;14(1):28–30. Available in: http://www.signavitae.com/wp-content/uploads/2018/03/SIGNA-VITAE-2018-14SUPPL1-28-30.pdf
7. Wilkinson I.B., Hall I.R., MacCallum H et al. Pulse-wave analysis: Clinical evaluation of a noninvasive, widely applicable method for assessing endothelial function.Arterioscler. Thromb. Vasc. Biol. 2002;22:147–152. Available in: https://www.ncbi.nlm.nih.gov/pubmed/11788475
8. Lane HA, Smith JC, Davies JS. Noninvasive assessment of preclinical atherosclerosis. Vasc Health Risk Manag. 2006;2(1):19–30. Available in: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1993970/
9. Sutton-Tyrrell K1, Najjar SS, Boudreau. Elevated aortic pulse wave velocity, a marker of arterial stiffness, predicts cardiovascular events in well-functioning older adults. Circulation. 2005 Jun 28;111(25):3384-90. Available in: https://doi.org/10.1161/CIRCULATIONAHA.104.483628
10. Wilmer W. Nichols, Clinical measurement of arterial stiffness obtained from noninvasive pressure waveforms. American Journal of Hypertension, Volume 18, Issue S1, January 2005, Pages 3S–10S, https://doi.org/10.1016/j.amjhyper.2004.10.009
11. Krantz et al. Pulse wave velocity and carotid atherosclerosis in White and Latino patients with hypertension.BMC Cardiovascular Disorders 2011, 11:15. Available in: http://www.biomedcentral.com/1471-2261/11/15
12. Terai M, Ohishi M, Ito N, Takagi T et al. Comparison of arterial functional evaluations as a predictor of cardiovascular events in hypertensive patients: the Non-Invasive Atherosclerotic Evaluation in Hypertension (NOAH) study.Hypertens Res. 2008 Jun;31(6):1135-45. Available in: https://www.ncbi.nlm.nih.gov/pubmed/18716361
13. M Jadhav, UdayN,KadamN. Non-invasive assessment of arterial stiffness by pulse-wave velocity correlates with endothelial dysfunction. Indian heart journal. 57. 226-32. Available in: https://www.ncbi.nlm.nih.gov/pubmed/16196179
14. Kim H-L, Kim S-H (2019) Pulse Wave Velocity in Atherosclerosis. Front. Cardiovasc. Med. 6:41. Available in: https://www.frontiersin.org/articles/10.3389/fcvm.2019.00041/full
15. Mceniery, Carmel & WallaceSharon et al. Endothelial function is associated with pulse pressure, pulse wave velocity, and augmentation index in healthy humans. Hypertension. 48. 602-8. Available in: https://doi.org/10.1161/01.HYP.0000239206.64270.5f
6. Vamsi V, Golub A, Pezić M, Fekete P, Findri P, Prkačin I. Presión arterial central y velocidad de la onda del pulso en pacientes con hipertensión resistente. Signa Vitae. 2018; 14 (1): 28-30. Consultado el 20 de agosto de 2019. Disponible en: http://www.signavitae.com/wp-content/uploads/2018/03/SIGNA-VITAE-2018-14SUPPL1-28-30.pdf [ Links ]
7. Wilkinson IB, Hall IR, MacCallum H et al . Análisis de ondas de pulso: evaluación clínica de un método no invasivo y ampliamente aplicable para evaluar la función endotelial. Arterioscler. Trombo Vasc. Biol. 2002; 22: 147–52. Consultado el 28 de agosto de 2019. Disponible en: https://www.ncbi.nlm.nih.gov/pubmed/11788475
8. Carril HA, Smith JC, Davies JS. Evaluación no invasiva de la aterosclerosis preclínica. Vasc Health Risk Manag. 2006; 2 (1): 19-30. Consultado el 17 de agosto de 2019. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1993970/ [ Links ]
9. Sutton-Tyrrell K1, Najjar SS, Boudreau . La velocidad elevada de la onda del pulso aórtico, un marcador de rigidez arterial, predice eventos cardiovasculares en adultos mayores que funcionan bien . Circulación. 28 de junio de 2005; 111 (25): 3384-90. Consultado el 18 de agosto de 2019. Disponible en: https://doi.org/10.1161/CIRCULATIONAHA.104.483628
10. Wilmer W. Nichols, Medición clínica de la rigidez arterial obtenida de formas de onda de presión no invasivas . American Journal of Hypertension, Volumen 18, Número S1, enero de 2005, páginas 3S – 10S . Consultado el 28 de agosto de 2019. Disponible en: https://doi.org/10.1016/j.amjhyper.2004.10.009
11. Krantz y col. Velocidad de la onda del pulso y aterosclerosis carotídea en pacientes blancos y latinos con hipertensión. Trastornos cardiovasculares BMC 2011, 11: 5 . Consultado el 20 de agosto de 2019. Disponible en: http://www.biomedcentral.com/1471-2261/11/15
12. Terai M, Ohishi M, Ito N, Takagi T et al. Comparación de las evaluaciones funcionales arteriales como predictor de eventos cardiovasculares en pacientes hipertensos: el estudio de evaluación no invasiva de la aterosclerosis en la hipertensión (NOAH). Hypertens Res. Junio de 2008; 31 (6): 1135-45. Consultado el 23 de agosto de 2019. Disponible en: https://www.ncbi.nlm.nih.gov/pubmed/18716361 [ Links ]










 texto en
texto en