Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Revista Científica Ciencia Médica
Print version ISSN 2077-3323
Rev Cient Cienc Méd vol.21 no.1 Cochabamba 2018
Original article
FRECUENCY OF BARRET'S ESOPHAGUS FOR GASTROESOPHAGEAL REFLUX IN THE CENTRAL UNIVERSITY OF VENEZUELA.
Cuauro Ruíz Gabriela1, Díaz Arreaza Dilia1, Ruíz Gómez María Elena1, Merheb Luttinger Michelle1, Malpica Pittol Alisson1
1Dra. Dilia Díaz Arreaza Gastrointestinal and Liver Section Director “Dr. Pedro Grases” Anatomopathological Institute “Dr. José A O´Daly”. Central University of Venezuela. Caracas.
Correspondence to: Dra. Dilia Díaz Arreaza E-mail: diliacda@gmail.com Telf. & celular: +58 414 7910032
Received for publication: October, 4 2017
Accepted for publication: July, 14 2018
Cite as: Rev Cient Cienc Med 2018;21(1):21-29
ABSTRACT
Introduction: Reflux disease develops when gastric content causes esophageal and extra esophageal symptoms and/ or complications. The esophageal complications include reflux, reflux esophagitis and Barrett's esophagus. The last is a pre-malignant condition characterized by a specialized intestinal metaphase whose importance lies in the knowledge of dysplasia due to its evolution to cancer. Previous investigations determined the prevalence of: dysplasia in Barrett's esophagus 33,3%; non erosive reflux disease 82,70% and erosive 17,30%; esophagitis with endoscopic and morphologic findings 84,37%.
Objective: To evaluate the prevalence of Barrett's esophagus in patients with reflux and reflux esophagitis in the Anatomopathologic Institute of Universidad Central de Venezuela.
Method: A descriptive and retrospective study was conducted. There were evaluated the esophageal endoscopic biopsies between 2005-2015, with diagnosis of reflux and reflux esophagitis. The presence or absence of dysplasia was reviewed in the Barrett's esophagus cases, with the respective grade. Absolute and relative frequencies were obtained by a descriptive analysis.
Results: 35,85% of cases were reflux and 64,12% were reflux esophagitis, both with women predominance and the average age was 55,2 and 53,1 years respectively. Eighteen cases (8%) with Barrett's esophagus were related to reflux disease. Low grade dysplasia represented 5,55%, indefinite for dysplasia 50% and negative for dysplasia 44,44%.
Conclusions: The prevalence of Barrett's esophagus associated with gastroesophageal reflux disease was 8%. The highest frequency was in the female sex with 66,66%, and the ages between 30 and 78 years with an average of 59,25 years.
Keywords: Biopsy, esophagus, reflux esophagitis, Barrett esophagus, cancer
INTRODUCTION
Reflux disease is a condition that occurs when gastric contents cause symptoms of heartburn, regurgitations and esophagus and extraesophagus complications1,2. Reflux is one of the esophagus complication, it characterized for stratified squamous epithelium with acanthosis and papillomatosis in two-thirds of esophagus surface, and more than 20% of basal cell hyperplasia. If these changes are associated with exocytosis of polimorphonuclears: neutrophils and eosinophils, reflux esophagitis is diagnosed3,4. They're necessary endoscopy and histopathological procedures to diagnose inflammatory disorders of the esophagus as Gastroesophageal Reflux (GER), Gastroesophageal Reflux Disease (GERD) and Barrett's esophagus5. It's known that gastroesophageal junction is usually symmetric and abrupt, histologically non keratinized stratified squamous epithelium differentiates from cylindrical relating to glandular epithelium. If it's observed gastric mucosa under esophageal epithelium, we are seeing columnar metaplasia6. It's important to recognize epithelial hybrid cells to distinguish esophageal from gastric epithelium and see in the low part of squamous epithelium the mucosa columnar cells, which is an adaptive change, being a precursor of Barrett's esophagus5.
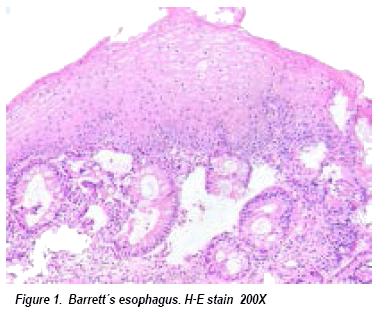
Barrett's esophagus is a premalignant condition, defined as the substitution of normal esophageal epithelium for specialized columnar metaplasia due to goblet cells presence (see imagen 1)7,8. Most clinical and experimental evidences indicate metaplasia results from chronic gastroesophageal reflux that lead to inflammation, mucosal ulcer, and subjacent reepithelization stem cells in situ, as a consequence, reflux causes a low Ph which make it differentiate into columnar metaplasia as an adaptive process4. The diagnosis should fulfill two criteria: endoscopic and histological. The first one is the observation of the squamocolumnare transition zone proximal to esophagus distal, characterized by a bright reddish smooth epithelium, juxtaposed on a whitish squamous stratified cells, above the Z-line corresponding to the squamocolumnare junction9.
The second criterion refers to histological findings already mentioned10. It's important to recognize dysplasia in Barrett's esophagus because It can progress to cancer, that's why exist the 1988 Consensus, which classifies dysplasia into categories as indefinite, negative, low-grade, high-grade that must be specified in the pathology report5,11,12. Previous studies performed by Garcia in the Anatomopathological Institute of Universidad Central de Venezuela during 1995 to 1999, they were investigated 266 cases of reflux esophagitis and Barrett's esophagus, determining dysplasia in 33,3%13. A paper by Poleo in 2010, related to the prevalence of GERD in two samples of Venezuelan people, this resulted in nonerosive GERD with 82,70% and erosive GERD with 17,30%14. A recent study of 2011 byCedeñoetal, studied reflux esophagitis with histological diagnostic and clinical and endoscopic variables; according to The Los Angeles Classification, the prevalence of esophagitis grade A and B with histological and endoscopic findings were 84,37 % 15. Due to previous studies, the purpose of this study was to assess the prevalence of Barrett's esophagus in patients with reflux and GERD in the Anatomopathological Institute "Dr. José A O' Daly"of Universidad Central de Venezuela.
MATERIALS AND METHODS
It was performed a cross-sectional, descriptive and retrospective study in the section of gastrointestinal and liver pathology Dr. Pedro Grases"del Instituto Anatomopatológico "Dr. José A O' Daly"of Universidad Central de Venezuela, 702 endoscopic samples of esophagus biopsies were examined during the 2005-2015 period. The pathology reports were reviewed including the diagnosis of reflux and esophagitis reflux that had histological specimens and paraffin tissue blocks available.
Furthermore, we review the biopsy enquiry forms of 702 patients, and obtained clinical information: sex and age. They were excluded samples with no database and the ones no gender or age could be stablished. 233 biopsies complied inclusion criteria whose specimens were observed using an Olympus® Cx 31 microscope by two specialist pathologists who supported the diagnosis.
It was assessed the absence or presence of dysplasia in Barrett's esophagus and its different categories. The collection data was made in the Excel® table taking into account the case number, age, sex, reflux, reflux esophagitis, Barrett's esophagus, Negative for Dysplasia, indefinite for dysplasia, low-grade and high-grade dysplasia.
It was obtained the number of cases with reflux and reflux esophagitis, we determined the average age and sex distribution. We associated each pathology with Barrett's esophagus as a consequence we got a frequency that quantifies the proportion of individuals who had illness during a specific time. All patients signed the consent informed for the biopsy, and data were assigned alphanumeric codes. In respect to patient's autonomy, there were no interference that involves their health and social welfare in compliance with ethical rules.
RESULTS
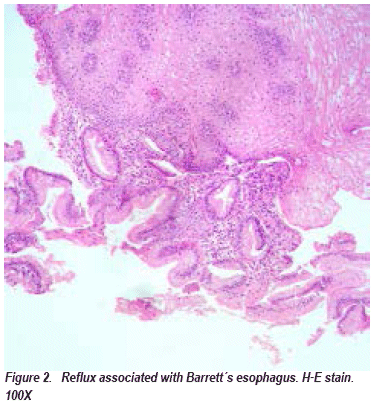
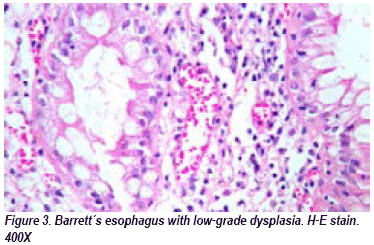
702 endoscopic biopsies of esophagus were reviewed in ten years, from which 223 (31,76%) cases complied inclusion criteria. Among the total of patients who were entered into the study, eighty (35,85%) had reflux and 143 (64,12%) reflux esophagitis. The age at diagnosis is an average of 55,21 years, being the minor a 1-year-old and the major a 81 -year-old patient. The sex distribution was higher in female with 42 patients (52,5%). Nine cases were associated with Barrett's esophagus (see figure 2), seven women and two men between 30 to 78 years old and an average age of 57. It was observed low-grade dysplasia in one patient (see Figure 3), four belonged to indefinite of dysplasia category and four were negative.
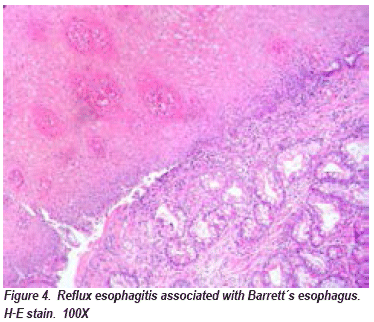
The reflux esophagitis had an average age of 53,14, the minor was 1-year-old and the major was 78-year-old. 86 female sex cases (60,13%) against 57 male (39,86%). Nine cases were associated with Barrett's esophagus (see Fig. 4), of which the predominating proportion was female sex with 5 patients between 56 and 73 years old, and an average age of 64. Four belongs to indefinite of dysplasia and five were negative.
A total of eighteen cases 8% of Barrett's esophagus caused by reflux disease were diagnosed. One case of low-grade dysplasia (5,55%), nine (50%) as indefinite of dysplasia and 8 cases (44,44%) were negative. The higher frequency was female sex with 12 patients (66,66%), male sex with 6 patients (33,33%) between 30 to 78 years old and an average age of 59,25.
DISCUSSION
Studies carried out in North America, show around 20 to 25% of patients have Gastroesophageal reflux disease, however in the Histopathological Institute of Universidad Central de Venezuela was 31,76% in ten years16. A recent study performed by Cedeño et al, obtained 84,37% of prevalence of esophagitis with endoscopic and histological findings . Gastroesophageal reflux disease is a common condition in adults, having more incidence in women and increase with age17,18.
As Poleo reported on his study, the prevalence of GERD in the group A, formed by 337 people with an average age of 50,9 years old, from which 62,87% were women using clinical factors to make a diagnosis and the group B of 335 people with an average age of 50,6 years old, from which 55,49% were women had medical history, esophagogastroduodenoscopy, and the biopsy of esophagus, all resulted in 17,30% of erosive and nonerosive esophagitis. In our study, the female sex and the age of presentation are similar. While in 2013 a published study about reflux and esophagitis reflux factors in 10 837 patients of Japan, it evidenced that men had more reflux esophagitis with 9,8% than women with 2,4% while reflux cases are more frequent in women 17,1 % than men 15,1 % 2. Unlike our study shows female sex has higher incidence in both pathologies.
Barrett's esophagus is associated with persistent ERG diagnosed in 10-15% of patients with GERD17,19. However, other study evidenced Barrett's esophagus was related to GERD in 6-12% of cases. Corresponding with our study, it identified 18 cases from 223, an incidence of 8%, which associates GERD to Barrett's esophagus17.
In 1995-1999, a study performed by our institution, 266 cases of GERD and Barrett's esophagus were selected and obtained the average age of 54, who had Barrett's esophagus, an increased incidence in male sex of 62%, and 66,7% negative for Dysplasia13. In contrast to this study, female sex was predominant with 12 cases, an average age of 59 and indefinite for dysplasia prevailed in 50% of patients.
The patients with Barrett's esophagus, only a minority develops cancer (0,5%), found at around 0,3% per year lately19,20. Many upper gastrointestinal diseases are increasing and require biopsy for their diagnostic. The upper endoscopic is an effective procedure to diagnose and control the evolution of GERD to Barrett's esophagus. It's also very important the prevention of serious complications: Barrett's esophagus that can progress to low-grade dysplasia, high-grade dysplasia and adenocarcinoma, in patients with gastroesophageal reflux20,21.
A limitation of this study was misinformation about clinical endoscopy that is necessary to make a correct diagnostic of Barrett's esophagus.
In conclusion, this study reports an incidence of 8% of Barrett's esophagus associated with GERD in the section of gastrointestinal and liver pathology, "Dr. Pedro Grases" of Instituto Anatomopatológico "Dr. José A O'Daly"de la Universidad Central de Venezuela. There was 5,5% of low-grade dysplasia; it was more frequent in women (66,66%) between 30 to 78 years old with an average age of 59,25%.
Recommendations:
We consider our study should build upon these findings in order to extend and get a better correlation and prevalence of these pathologies.
REFERENCES
1. Vakil N, Van Zanten SV, Kahrilas P, Dent J, Jones R; Global Consensus Group: The Montreal definition and classification of gastroesophageal reflux disease: a global evidencebasedconsensus. Am J Gastroenterol [Internet]. 2006 August [Citado jul 2016];101(8):1900-20. Disponible en: https://www.ncbi.nlm.nih.gov/pubmed/16928254
2. Chihiro M, Takeshi S, Hikaru K, Yu T, Mitsuhiro F, Yoshiki S. Background Factors of Reflux Esophagitis and Non-Erosive Reflux Disease: a cross-sectional study of 10,837 subjects in Japan. Plos one [internet]. Jul 2013 [Citado 10 jul 2016];8(7):e69891. Disponible en: http://journals.plos.org/plosone/article?id=10.1371/journal. pone.0069891
3. Rui- Hua W. From reflux esophagitis to Barrett’s esophagus and esophageal adenocarcinoma. World J Gastroenterol [internet]. May 2015 [Citado 15 jul 2016]; 21(17): 5210-5219. Disponible en: https://www.wjgnet.com/1 007-9327/ full/v21/i17/5210.htm
4. Rosai and Ackerman. Patología quirúrgica. Tracto gastrointestinal. 10a ed. Nueva York: Amolca; 2011. p. 591.
5. Day D, Jass J, Price A, Shepherd N, Sloan J. Morson and Dawson’ s gastrointestinal pathology. 4th ed. USA: Blackwell; 2003. p. 38-43.
6. DenNrdi F, Riddell R. Histología para patólogos. Esófago. 3a ed. Colombia: Amolca; 2007.p. 585.
7. Taylor J, and Rubenstein JH. Meta-Analyses of the Effect of Symptoms of Gastroesophageal Reflux on the Risk of Barrett’s Esophagus. Am J Gastroenterol [Internet].2010 August [Citado 15 jul 2016];105:1730-37. Disponible en: http://www.nature.com/ajg/journal/v105/n8/full/ajg2010194a.html
8. Turner JR. Tubo Digestivo. En: Kumar V, Abbas A, Fausto N, Mitchell R. Robbins Patología Humana. 8a ed. España:Elsevier; 2010. p. 769-771
9. Cardoza J, Dib J. Esofago de Barrett, Hospital general Dr. Jesus Yerena. Revista Gen. 2013;67(1):42-48
10. González N, Parra-Blanco A, Cohen H. Esófago de Barrett. Acta Gastroenterológica Latinoamericana. Diciembre 2012;42(4).
11. Lacobuzio C, Montgomery E. Patología Hepática y Gastrointestinal. 2da ed: Elsevier;2012.
12. Tamayo-de la Cuesta JL. De la esofagitis al esófago de Barrett. Revista Gastroenterol Mex. 2005.70(1).
13. García M. Estudio clínico morfológico de esófago de barrett en biopsias de pacientes con esofagitis por reflujo 2001[Tesis]. Caracas: Universidad Central de Venezuela;2001.
14. Poleo J. La enfermedad por reflujo gastroesofágico: su prevalencia en dos muestras de población venezolana con referencia a la presencia de alteraciones endoscópicas y al valor de la biopsia esofágica en el diagnóstico de esta condición. Gen 2010;64(3).
15. Cedeño F, Castillo R, González H, Weber W, Hinestroza H, Wagner V. Esofagitis por reflujo diagnóstico histológico y su relación con variables clínicas y endoscópicas. Revista Gen [Internet]. octubre-diciembre 2011;65(4):310-312. Disponible en: http://www.genrevista.org/index.php/GEN/article/view/304/pdf
16. Moore M, Afaneh C, Benhuri Dl, Antonacci C, Abelson J, Zarnegar R. Gastroesophageal reflux disease: a review of surgical decision making. World J Gastrointest Surg [Internet]. Ene 2016 [Citado 16 jul 2016];8(1):77-83. Disponible en: https://www.wjgnet.com/1948-9366/coretip/v8/i1/77.htm
17. Daniele DO, O’Donnell FL, Clark LL. Incidence of gastroesophageal reflux disease (GERD), active component, U.S. Armed Forces, 2005-2014. MSMR [Internet]. Jul 2015 [Citado 20 jul 2016];22(7):14-7. Disponible en: https://www.ncbi.nlm.nih.gov/pubmed/26207411
18. Dickman R, MAradey-Romero C, Gingold-Belfer R, Fass R. Unmet Needs in the Treatment of Gastroesophageal Reflux Disease. J Neurogastroenterol Motil [Internet]. Jul 2015 [Citado 25 jul 2016];21(3):309-319. Disponible en: https://www.e-sciencecentral.org/articles/SC000011071
19. Bartlesman JF1, Hameeteman W, Tÿtgat GN. Barrett’s oesophagus. Eur J Cancer Prev [Internet]. Jun 1992 [Citado 28 jul 2016];1(4):323-5. Disponible en: https://www.ncbi.nlm.nih.gov/pubmed/1467782
20. Martinucci I, Bartoli N, Russo S, Bertani L, Furnari M, Mokrowiecka A. Barrett’s esofhagous in 2016: from pathophysiology to treatment. World J Gastrointest Pharmacol Ther [Internet]. Mayo 2016 [Citado 27 jul 2016];7(2):190-206. doi:10.4292/wjgpt.v7.i2.190. PMID:27158534; PMCID:pmc4848241.
21. Walker MM, Harris AK, Edwards GC, Talley NJ. A GP primer for understanding upper gastrointestinal tract biopsy reports. Aust Fam Physician[Internet]. Oct 2015 [Citado 27 jul 2016];44(10):706-11. Disponible en: https://www.ncbi.nlm.nih.gov/pubmed/26484483
6. DenNrdi F, Riddell R. Histología para patólogos. Esófago. 3a ed. Colombia: Amolca; 2007.p. 585. [ Links ]











 text in
text in